When famed HIV/AIDS doctor Howard Grossman unveiled data at an October 18 conference that showed a PrEP-adherent man had acquired the HIV virus despite taking the preventive drug, some panicked.
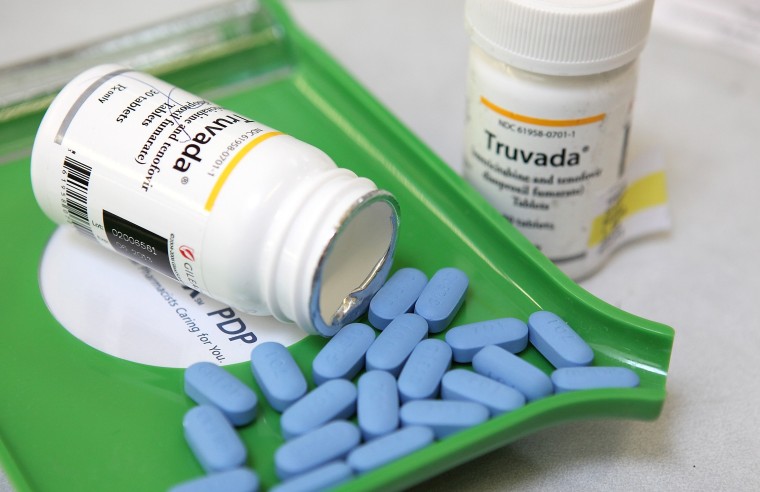
Headlines referred to the case as a “PrEP failure,” a “new drug-resistant HIV strain” and other scary terms that called into question the efficacy of Truvada—the HIV-prevention prophylactic medication that has been called a miracle drug in the fight against AIDS.
But according to experts interviewed by NBC OUT, the October case—the second known HIV transmission in a PrEP-using patient this year after a similar transmission occurred in Toronto this February—is neither the harbinger of a new doomsday virus nor an unexpected turn in the way PrEP is supposed to work.
“This is not an emergency,” Demetre Daskalakis, Assistant Commissioner of NYC’s Bureau of HIV/AIDS Prevention and Control, said. “This is an expected outcome in a really good prevention strategy. It’s one we can avert.”

Daskalakis, affectionately known in the HIV-prevention community as “Doctor D,” went from doing infectious disease research at Harvard to setting up STI testing clinics in gay nightclubs before becoming New York’s assistant HIV czar. As Daskalakis explained, there are two main reasons why the October case happened: the predictable mutability of the HIV virus itself and avoidable gaps in the individual’s prevention plan.
First, the virus: “When you have HIV up against medications that people might not be taking enough of, the virus will randomly replicate,” Daskalakis said. “The HIV that gets selected out ends up resistant to those drugs. We know this is what HIV does, and that’s why we do resistance testing to make sure the drugs match.”
And no, there is not a new “PrEP-resistant HIV strain.” As researchers have long known, there’s no one strain of HIV at all—the virus can, and does, mutate—which is why resistance testing is done on all cases. The testing is vital for HIV-negative partners of people living with the virus; if the HIV virus that one partner carries is shown not to be resistant to PrEP, the negative partner can take Truvada and have a negligible risk of contraction.
RELATED: New Study Shows HIV Epidemic Started in New York in 1970
But in order to know that PrEP is working against the virus, you need to know the exact virus you’re dealing with. And as Grossman explained in a detailed October 18 interview with TheBody.com, the October case showed that the failure had little to do with Truvada—and everything to do with testing and other HIV-prevention precautions such as condom use.
According to Grossman, the patient acquired a strain of the HIV virus that was different from the one his HIV-positive primary partner carries. The couple had engaged in condomless sex with people outside of the relationship—and the virus was contracted from one of the unknown partners.
"There is negligible risk of HIV transmission when a person has undetectable HIV viral load," Grossman told TheBody.com, pointing out that the HIV-positive primary partner has been undetectable since 2012. "With unknown partners of unknown HIV status who might not be well controlled and might have a resistant virus—there's the risk.”
Approximately 100,000 people are currently taking Truvada, according to Grossman. Two cases of transmission out of that number is a very low rate—especially when circumstantial mistakes are factored in. And while PrEP has been touted as a miracle, doctors have consistently maintained that it doesn’t have a 100 percent success rate. But with millions of new HIV transmissions per year across the world, drugs like Truvada are still poised to radically transform prevention. That is, if people can get to them.
Jason Walker, a community HIV/AIDS organizer with VOCAL-NY, told NBC OUT that access to PrEP is a much bigger problem than the .002 percent of HIV transmissions occurring among current users.
“We see ads [for PrEP] everywhere in New York, but there’s still low-income communities of color and people without insurance who are still unable to access the medication,” Walker said. “Black men who sleep with men experience HIV transmission at high rates but are the lowest on PrEP treatment.”
Drugs like Truvada are just new enough that outreach and education are still needed to reach the communities most affected by HIV, like transgender women, black men who sleep with men and low-income drug users. But even among those groups, people sometimes brush off PrEP as an option they can’t afford without health insurance—not realizing that strong programs exist to cover the cost of the drug.
Gilead, the pharmaceutical company that manufactures Truvada, has an in-house coverage program that operates somewhat like a PrEP scholarship. On social media, PrEP users frequently refer to the “Gilead card” as the holy grail of reduced (or free) prescription cost.
In addition to the Gilead card, non-profits like the Patient Advocacy Foundation and medication assistance programs (MAPs) can cover the cost of Truvada prescriptions for at-risk people who lack insurance.
But as Walker pointed out, popping the little blue pill every day isn’t the only way to stop HIV.
“The issue is the person who passed on the virus who was not undetectable. That person was not getting proper treatment,” Walker said. “There needs to be more work in identifying who’s infected so that we can achieve viral suppression. These incidents aren’t about PrEP, they’re about what we’re doing to find folks who are positive and are not accessing treatment.”
RELATED: AIDS Activist Larry Kramer on 'Patient Zero' Myth, HIV Stigma
Unless you know the status and viral resistance of every single person you have sex with, PrEP alone isn’t going to cut it—condom use is still necessary, too. The October case surprised some in the gay community who believed that “tops” (men who have insertive, rather than receptive, sex with other men) cannot acquire the HIV virus. But anyone on PrEP can get HIV if they don’t use condoms with partners whose viral status is unclear.
As Daskalakis pointed out, even the two cases of HIV transmission in PrEP-adherent men worked out about as well as can be expected. In the October case, the virus was detected and treated so quickly, the man was immediately undetectable—meaning the viral count in his blood is so low that passing on the virus to anyone is highly unlikely.
“A positive HIV result is not bad news. The only bad news is no news at all,” Daskalakis said. “This guy’s prevention plan was pretty good—and even pretty good can slip up. But to acquire HIV and five minutes later be undetectable, it’s great. HIV is just an infection, and that’s how we treat it now. It’s not special.”
EDITOR'S NOTE: This article has been updated from its original version.