States that have refused to expand Medicaid, as requested as part of the Obamacare health reforms, say they can’t afford to cover all the old, sick people who will be just waiting to get their free health care.
But a new study contradicts this argument, saying the people who would become newly eligible for Medicaid are going to be younger white males who aren’t sick yet– but who are more likely to be smokers and drinkers who would benefit from getting medical care now.
“There are going to be many more males. They are going to be younger," says Dr. Tammy Chang of the University of Michigan, whose study is published in the Annals of Family Medicine.
This could mean that providing Medicaid to more people could cost less than forecast, Chang said. “They are using what the Medicaid population looks like now,” she said. But the study she did with colleague Dr. Matthew Davis shows those who will become eligible for Medicaid for the first time may be a healthier batch than the 50 million people who are now covered.
Medicaid, the state-federal health plan, provides minimal coverage in many states to those deemed in the most need of help. Pregnant women make up a large percentage in most states, as well as children and the very poor.
The 2010 Affordable Care Act was designed to transform health care in the United States, providing health insurance for just about everyone. The law required states to extend Medicaid to people earning up to about 138 percent of the federal poverty level, or about $14,800 for single people and $31,000 for a family of four.
In return, the law pledges that the federal government will pay 100 percent of the additional costs for the first three years of the program. States will have to kick in a very small percentage more each year after that.
But after a series of challenges to the law, the U.S. Supreme Court ruled in June 2012 that the Medicaid expansion requirement went too far. States can’t be forced to add more people to Medicaid, the court ruled.
Now the Congressional Budget Office projects that 13 million people will become newly eligible for Medicaid in the states that choose to expand their offerings by 2022. The non-profit Kaiser Family Foundation calculates this would cost states $8 billion more between now and 2022.
But it may be less. Chang and Davis looked at a large health survey called the National Health and Nutrition Examination Survey. Participants answer detailed questions about themselves, their health and their health coverage. They compared current Medicaid patients to people who would be eligible for the program based on income.
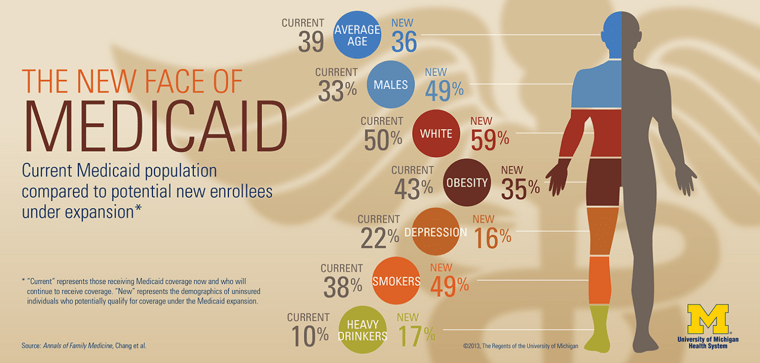
Currently, the average Medicaid patient is 38.7 years old. If all the states expanded Medicaid – and not all will – the average age would go down to 36.3. Right now a third of patients are male; under a full expansion, 49 percent would be. Right now, almost precisely half of beneficiaries are white; under the expansion, nearly 59 percent would be.
“Overall, potentially eligible adults are expected to have better health status (34.8 percent 'excellent' or 'very good,' 40.4 percent 'good') than current beneficiaries (33.5 percent 'excellent' or 'very good,' 31.6 percent, 'good',” they wrote.
Fewer would be obese and fewer would be depressed. But more would be smokers and heavy drinkers. Because these potential patients said their health was good, this could mean there’s an opportunity for doctors to help them stop smoking and cut back on their drinking before they do get sick, Chang says.
According to the Advisory Board Company, 24 states plan to expand Medicaid to more people and four states are leaning that way. Sixteen are definitely not and another seven probably won’t.