Pick up a newspaper, turn on the TV and it’s there: the news about avian flu.
It can be alarming sometimes, often confusing. And nearly everyone has the same question: Could it happen here?
In a special Dateline, the world’s top flu experts helped us create a dramatic vision of how our world might change in the grip of a pandemic.
Some background
In 1996, a new and particularly deadly strain of avian flu was found in a goose in China. It was found a year later in Hong Kong and six people died from the virus. They were the first known human cases.
But in 2003, this same deadly strain of virus appeared again in bird populations and this time it spread rapidly—through China and into Southeast Asia.
It spread, according to experts, by migrating water fowl and by the legal and illegal trafficking of birds and bird parts.
From Southeast Asia, the virus moved into remote sections of Russia, then into Central Europe. In the last several months, it has spread to parts of Africa and Western Europe.
Almost 200 people are known to have been infected in 9 different countries. More than half of them have died.
As far as we know, the people infected with the current strain of avian flu did NOT get the virus from another person but after extremely close contact with sick birds—and even those cases are rare.
Experts say this deadly virus could infect birds here in the U.S. in a matter of months.
“People are concerned about poultry, but they don’t need to be if, in fact, they cook it. If it’s well cooked, it’s safe to eat and you’re not going get the avian flu,” says Dr. Sue Bailey, Former Assistant Secretary of Defense for Health Affairs.
But here’s the bigger worry: The avian flu virus is constantly mutating and what is keeping health experts up nights is the possibility that it might change into a virus that can be easily passed from human to human.
And that could trigger a pandemic, the uncontrollable global spread of a disease. No one knows when, how or even if it will happen. But the world’s top flu experts are telling us to prepare.
We’ve had three pandemics in the last century— including the big one: the so-called Spanish Flu of 1918 that killed up to 40 million people worldwide and more than 500,000 Americans. People were afraid to go outside. There were shortages of food and medical supplies.
Will history repeat itself?
Secretary of Health and Human Services Mike Leavitt is the man charged with preparing America for the next pandemic.
“Anything we say before a pandemic happens feels alarmist,” says Leavitt. “Anything that we have done once a pandemic starts seems inadequate. We’re at a greater risk of a pandemic than at any time in decades. We are overdue. And we’re under prepared.”
To prepare this report, we’ve consulted with the men and women who will be on the front lines of a pandemic if it were to happen—experts from international, federal, state, local agencies and many more.
They have given us their views, predictions and their guidance.
On Sunday night, Dateline took an unusual step to illustrate what the future might hold. Using doctors, medical students, actors and volunteers, we’ve produced a scenario based on what those experts say could happen in a world threatened by pandemic.
What you’re about to see is not intended to frighten or alarm—but simply to ask the question.... are we prepared?
“You and I are sitting on the crater of a volcano that’s pretty active, and the gas is coming out of little holes. It’s bubbling underneath our feet. ” Dr. David Nabarro, United Nations coordinator for Human and Avian Influenza.“We just don’t know when it’s gonna blow.”
Day one. This scenario starts on a Friday during flu season. It would be a busy night in the Emergency Department of a large hospital in New York City. A woman is brought in by her husband. He tells the triage nurse that his wife has been feeling ill for the past couple of days; a fever, cough, sore throat.
“Based on her symptoms alone—having the flu in the middle of flu season is not going to be unusual,” says New York City Department of Health’s Dr. Isaac Weisfuse.
“She will look like dozens of other patients, maybe hundreds of other patients that the triage nurse has seen that day,” says Dr. Eric Toner of the Center for Biosecurity, University of Pittsburgh Medical Center, who has been involved in hospital disaster planning for more than 20 years.
It is so busy, the woman would be forced to wait for more than an hour before she is seen by a doctor. Though no one would know it, the woman is infected with a new flu virus that could change the lives of everyone—not just in New York City, but in the entire world.

As she coughs she would spread millions of copies of a newly-mutated virus that is deadly, and passes easily from one human to another.
“Everybody who walks by, everybody sitting next to her will be exposed to the virus. Now most of them won’t get sick, but some will.”
“They have a fever, a cough. They’ll feel achy. And they’ll experience shortness of breath,” describes Dr. Toner. “Probably, she’ll get a chest x-ray, which would likely show evidence of pneumonia.”
She could be one of thousands of cases of pneumonia in New York City every year.
“She would not stand out at this point,” Dr. Toner adds.
Day two. In this scenario, the patient suddenly stops breathing— another indication to doctors that she might have a severe case of pneumonia. A hospital team would try to revive her.
When they get her breathing again, she would be placed on a ventilator. Doctors might still believe she had pneumonia, and would try to learn more about their patient.
In this scenario, the patient’s husband tells the nurse his wife travels often for business and that she recently flew from Vietnam to Hong Kong, then to Los Angeles. She was in Seattle for more business meetings, and then home to New York.
But it’s that visit to Vietnam where, in recent years, some have fallen ill and died of the avian flu: that would be the most significant information for the doctors in New York.
“That, in an astute clinician, should trigger the thinking that maybe this is the beginning of something,” says Toner.
Given the woman’s steep decline, and the knowledge of her recent travel to an avian flu “hot zone,” they would call the New York City Health Department. Officials there would ask more questions.
“We’d start at the beginning: How many days did she spend in every country? Where did she spend her time? Was it in the big city? Was it in rural areas?” says Dr. Isaac Weisfuse of the questions they would ask.
The hospital would then send samples from the woman to a lab for testing. New York investigators would call their colleagues at the CDC in Atlanta, who would then shift into high gear.
“We would use our authority to request a manifest from the airline,” says Dr. Martin Cetron, director for Global Migration and Quarantine at the CDC. They would try to identify all the flights the businesswoman took, where she sat, and who she sat next to, to find out if anyone else is sick.
“These are exposures may have occurred in airports with thousands of people aggregating. You may be behind the eight ball right from the very beginning,” says Dr. Cetron.
In this scenario, the woman in New York, like a lot of international travelers, has been on four flights in less than a week.
“That’s an enormous challenge, in fact of getting accurate contact information to swiftly identify people. And so it’s a race against the clock, really,” he says.
Day three. The New York woman’s lab results would be back. By now, the CDC would confirm that she is infected with a virus similar to the avian flu. But even the lab wouldn’t be able to answer the most important question: Did she get it from a sick bird, or from another person?
New York City officials wouldn’t know either. But because reports of a bird flu case could cause panic, they would probably hold a news conference to tell the public there was no need for alarm at this point.
Day four. A worldwide effort would be launched to determine if the New York City case is evidence of human-to-human transmission.
Scientists at the CDC would have by now contacted their colleagues at the World Health Organization in Geneva, Switzerland.
There, Dr. Mike Ryan is the man in charge of monitoring infectious disease outbreaks around the world.
“We pick up information on suspect human cases of avian influenza every day. Any one of those cases could represent the emergence of a pandemic strain,” Dr. Michael Ryan, Dir. of Epidemic and Pandemic Alert and Response at WHO.
In our scenario, the World Health Organization is investigating a small number of cases of avian flu in Vietnam, but there is no confirmation of human to human transmission.
“If we found out that there was a cluster of cases in Vietnam, this would be an immediate red flag,” says Dr. Nancy Cox, the chief of the Influenza Branch of the CDC. “Our patient had traveled from Vietnam.”
With no way of knowing whether she caught the virus from a bird or a human, the CDC would issue a Health Alert to hospitals and health care workers around the country alerting them to the New York case.
Without knowing exactly what virus they are even dealing with, doctors can’t save the businesswoman.
But at this point in our scenario, no health official would know enough to declare a pandemic.
“There’s no documented evidence of sustained human-to-human transmission. That’s what you’re looking for in order to declare a pandemic,” says Dr. Cox.
All that would be about to change.
In Dateline's scenario, one fatally sick traveler has set off a chain reaction among medical investigators around the world. Have their worst fears come to pass? Did she have a mutant form of avian flu that could trigger a pandemic?
“An influenza pandemic is like a brush fire. It will not stop at a street. It will jump over a brook. It will travel globally. And its damages will travel globally,” says Dr. Klaus Stohr, senior advisor on influenza pandemic vaccine development.
In this scenario, a businesswoman in New York City has died from a strain of avian flu. But at first, no one would declare a pandemic because doctors would have no way of knowing the virus that killed her could pass easily from human to human.
Day five. CDC investigators would now be tracing the travel history of that New York patient to find everyone who came into contact with her.
“There’s a group of people that are clearly at risk,” says Dr. Martin Cetron,Director for Global Migrations and Quarantine at the CDC. “They need to be found quickly.”
Health officials would be holding their breath.

“We are all sitting around the table and saying, ‘Where is the next case going to be?’ and what’s the move on the chess table when the second case pops up?” he adds.
In the scenario it happens: That same day in Davenport, Iowa, a sick young man is taken to his local hospital emergency room. He’s weak and has a fever.
Because of the CDC’s alert, hospital workers would know to be cautious and wear masks & protective gowns.
“We’ll take them back to our treatment area and away from other patients, get them out of the waiting room as soon as possible to decrease the risk of exposure to other people,” says Lisa Caffery, Epidemiology Project Coordinator at Davenport’s Genesis Medical Center.
The triage nurse would know to ask him about his travel history.
The man in this scenario lives and works in Los Angeles. After flying to Seattle for business, he went on to Iowa to attend a reunion.
He hasn’t traveled outside the U.S. in years, but his symptoms and the fact that he was recently on a plane would be cause enough for local officials to call the CDC.
Investigators would also try to contact people who were at the reunion.
2,000 miles away from Iowa, in Seattle, Washington, a woman is waiting to see her doctor and she’s feeling sick. Because of the CDC’s warnings and the media coverage, the physician here would know about the woman in New York City.
“If someone is critically ill, they’d be referred to a hospital,” says Dr. Jeff Duchin, Chief of the Communicable Disease Control Epidemiology and Immunization Section at Public Health, Seattle-King County. “Hopefully, everybody will understand the precautions that need to be taken.”
The doctor here does take precautions and get the woman to the hospital. The woman tells doctors she’s a flight attendant, working a commuter run between Seattle and Los Angeles, but hasn’t been out of the country in months.
But since she is a flight attendant, doctors would worry about a connection to the New York City case.

They would send samples to a lab, and call the Centers for Disease Control and Prevention. It would be the third report the CDC has received in less than a week. Officials would begin to fear the worst.
“That’s a bad sign. We’re gonna go back to get the itineraries of the Davenport case and the Seattle case. And it will not surprise anyone if there’s an overlapping leg somewhere, where two of those people are on the same flight manifest,” says Dr. Cetron.
Day six. In our scenario, both patients in Davenport, Iowa and in Seattle are infected with the same strain of virus that killed the business woman in New York.
Now health officials would have to figure out how the three cases, thousands of miles apart, could be related.
Doctors give the flight attendant in Seattle the anti-viral Tamiflu from the hospital’s limited supply.
Tamiflu has been effective in some cases of the avian flu, but has never been used against a pandemic strain.
Meanwhile, the patient in Davenport continues to decline.
Day seven. It could take this long for investigators at the CDC to confirm the worst: that the cases in New York, Davenport and Seattle are related.
In the scenario, all three were on the same flight from Los Angeles to Seattle. The Davenport patient sat next to the businesswoman from New York, who had just returned from a trip to Vietnam. The flight attendant was on that plane.
The CDC says this would be the critical piece of information they had been looking for, but hoped they’d never find—evidence of human-to-human transmission.
“Those are all the pieces of the puzzle that come together that make for a very worrisome scenario. We now have a cluster that really looks like human to human spread of a novel influenza virus— a worrisome finding,” says Cetron.
Health officials would now know, they are seeing the beginning of a pandemic.
Scientists at the World Health Organization would be seeing more human cases in Vietnam, where the New York woman had traveled.
The WHO would likely deploy a rapid response team to the region. The team would distribute anti-virals, and implement quarantine measures. To be effective, they would have to respond within just a few weeks of the first case.
“We do believe that if we were to react quickly enough to such a scenario, we could possibly slow down or stop the emergence of a pandemic strain,” says Dr. Mike Ryan.
“However, we say slow down and we say the chances of stopping it are unknown.”
By now, health officials in the U.S. would likely be informing the public that a pandemic had started. Since they would have identified and isolated the new virus, scientists could begin to take the first steps in the long process of developing a vaccine.
“It’s going to require at least six months before we get vaccine out the other end of the pipeline—any vaccine,” saysDr. D.A. Henderson, Center for BioSecurity, University of Pittsburgh Medical Center.
Investigators would also be engaged in an almost-impossible task: trying to find the thousands of people who may have had contact with the three patients.
Day 13. Anyone who came into close contact with any of the patients could now be infected. That’s because flu viruses can spread rapidly and easily from person to person.
“Influenza viruses are very successful viruses per se. They cause coughing and sneezing. And that allows a virus to be spread from person to person,” says Dr. Nancy Cox, Chief of Influenza Branch of the CDC.
A flu virus enters the body after being breathed in. It heads to the lungs, latching on to the cells inside, and then squirts genetic material into the cell, making copies of itself. That kills the cell, which then bursts open and spews millions of new viruses into the victim.
Some are coughed out, infecting others. The rest are attacked by the body’s immune system.
It’s the body’s efforts to fight off the virus that causes most of the symptoms that make us feel bad--- aches, fever, coughing. But there’s an irony sometimes associated with a pandemic flu virus: the healthier you are, the sicker you could become. During the 1918 pandemic, young adults were the hardest hit. Their dynamic immune systems often overreacted, and turned deadly.
“In a virus which is particularly virulent, this immune response can inflame the lungs to such an extent that the lung is filled with bloody fluid and basically the patient dies of drowning,” says Dr. Toner.
Back in our scenario, two people who came into contact with the businesswoman are now sick: a person who sat next to her in the waiting room and a nurse who tended to her.
“This is a bigger story than just our one case in New York City,” says Dr. Isaac Weisfuse. “I think it’s the warning flag to get ready.”
A hospital worker in Seattle is also sick, as is a person who attended the reunion in Davenport. Two restaurant workers at a truck stop just outside Davenport have also come down with the virus.
“We would expect that this virus would then result in many, many cases in multiple areas. There’s clusters in this country and that country,” Dr. Cetron.
In our scenario, the World Health Organization’s rapid response team, given the almost impossible odds, can’t contain the virus. Human cases would now be popping up in other Asian countries, beginning a march around the world.
Day 14. The flight attendant in Seattle is recovering, but the patient in Davenport has died.
Just two weeks after the woman in New York came to the hospital, the virus is spreading.
The virus now would be traveling from city to city and life for virtually all Americans would undergo a dramatic, and possibly devastating, change.
“People need to be prepared for the fact that, with a severe pandemic, there could be a lot of sick and dying people on top of our day to day demands placed on our health care system,” says medical anthropologist Dr. Monica Shoch-Spana.
Day 30. As the flu pandemic spreads. It would catch a lot of people by surprise.
“You might in the morning brush your teeth, listen to the radio and find out that the virus has hit your community. There will be no big changes for you in the first couple of days,” says Dr. Klaus Stohr is a senior advisor to the World Health Organization.
The virus begins to spread from the three cities first hit in our scenario: New York, Davenport, Seattle.
As it’s now passed from human to human, the virus would likely travel along interstate highways, and airline routes.
Scientists say each city and town would experience waves of infections that would peak after approximately five weeks. The virus would continue to spread randomly—across borders and time zones. And scientists say it could circle the globe as many as three times.
“So the first wave may come through and affect young families. The second wave may come through and affect the elderly, to a greater extent. And a third wave may come through and pick up those who haven’t been infected already,” says Dr. Nancy Cox.
Day 40. In many parts of the United States, this would now be the worst time— the peak of the pandemic.
Hospitals emergency rooms would be overwhelmed with patients.
“New York has a population of just under eight million,” says Dr. Martin Meltzer, a senior economist at the CDC, who helped design a computer program that predicts numbers of sick and dead during a pandemic.
Based on New York City’s numbers, here’s what might happen in that worst week: About 5,000 people arriving at New York City hospitals.
That’s 5,000 people in addition to other patients. He says the demand for ICU beds and ventilators in all three cities from our scenario would be impossible to meet.
“The scale of a severe flu pandemic will be so much greater than anything that you’ve ever seen before,” says Dr. Eric Toner, University of Pittsburgh’s Center for Biosecurity.
Today, many hospitals are economically strapped, and don’t have funds to stockpile medical supplies. So it would be no surprise, in a pandemic, if doctors run short.
“Hospital staff are stretched to the limit. And this has been going on for five weeks. This isn’t just a bad weekend,” says Martin Meltzer.
“We’ll have patients who are normally treated in an intensive care unit being treated in hallways,” says Dr. Toner. “There won’t be two nurses to one patient. Maybe there’ll be one nurse to five patients, if we’re lucky. And there will still be babies to be born. There will still be accidents. There will be cancer patients that are getting treated.”
Hospitals all around the world would be forced to cancel elective surgeries to make room for the influx of flu patients.
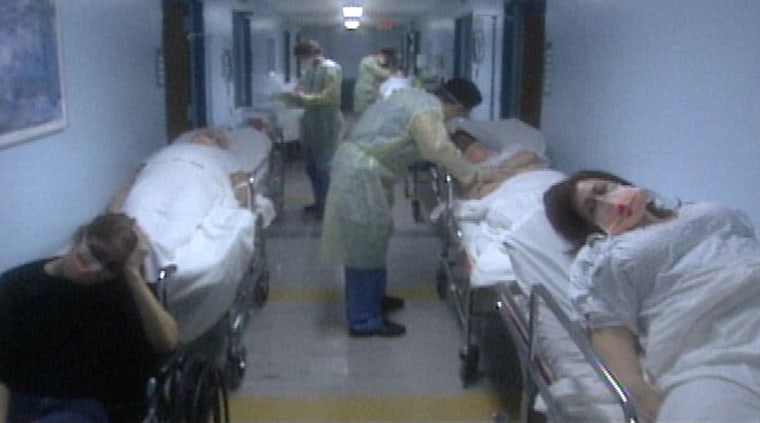
Regions hit with natural disasters would also be dealing with thousands of flu patients.
Countries struggling against AIDS would now be hit with another deadly virus.
Hospital workers would likely be affected more than anyone else. Many would be sick, and the others would be working around the clock in hospitals, and tending to their own sick families.
“Would I be afraid to go to work? You have to go through those questions individually. What about my kids?” says Dorothy Teeter, Director, Public Health, Seattle-King County, of the questions individuals have to ask of themselves.
“I have elderly parents and a son with diabetes. So, I have to be a little bit more concerned about that. Because I would be here. I have to learn to balance that,” says Lisa Caffery RN, and Epidemiology Project Coordinator, Davenport’s Genesis Medical Center.
Eventually, access to many hospitals might even be restricted.
Even for those who don’t get sick, life would change profoundly. Restaurants, bars, and stores would be empty.
“Entertainment, movie theaters and Broadway will close. They’ll have no business,” predicts Dr. Toner.
But despite the pressures to close, some places might stay open.
“There are some very famous photographs from 1918 where the authorities had banned church gatherings but people held an impromptu church service outside,” says Dr. Toner.
“You’ll have a disruption of things that we take for granted,” says Dr. Shoch-Spana. “Whether it’s trash pick up, mail delivery, or access to police officers.”
“Utilities break down, like electricity, or sanitation or water. There won’t be people to repair them. So there may be shortages of electricity,” says Dr. Nabarro.
Deliveries of goods to warehouses and grocery stores would slow down. It also takes people to drive the subways, buses and trucks. Service disruptions and spotty commuter service would be common all over the country.
Some experts estimate as much as 40 percent of the work force could be absent at any given time during the pandemic.
“Work places will become ghostly and companies won’t be able to function,” says Dr. Nabarro.
Health officials would recommend radical changes to try to control the spread of the virus and protect vulnerable populations like children.
“We’re talking about situations that increase social distancing. School closures, potentially workplace closures, and having families hunker down at home,” says Dr. Martin Cetron, Director For Global Migration And Quarantine at the CDC.
Public gatherings, like baseball games and concerts might be cancelled. There would be talk of quarantine, but not the kind many of us might envision.
“We’re not going to see this nightmare scenario of armed guards with ‘shoot to kill’ orders,” says Dr. Cetron. “A voluntary approach to staying at home, sheltering in place, taking care of yourself and your loved ones, leverages your instinct to do the right thing.”
“People need to be prepared for extraordinary events. But they also need to be prepared for a problem that takes a long time to unfold,” says Shoch-Spana.
In the end, how many would die? And how would we know when the pandemic is over?
The pandemic at its peak would devastate communities across America and the entire world.
It would touch virtually every one of us in some way. But how will we know that the worst is over — and what will the pandemic leave behind?
Day 75. The pandemic has passed its peak. The National Institutes of Health estimate that at this stage over one million Americans could be infected, and hundreds of thousands could be dying or already dead. But the country is learning to cope.
“The notion of a panicked public—it makes for a great story. It makes for great movies and books. But, in the end, most people are just trying to muddle through an extraordinary time.
“You’ll see people be a little bit more cautious,” Martin Meltzer, Sr. Health Economist, Office of Surveillance, National Center for Infectious Diseases, CDC. “People are unlikely to shake hands with strangers, or even people they know, unless they are fairly certain, for example, that that person isn’t infectious.”
Day 90. Three months into our scenario, people have been dealing with large numbers of sick and dead. Almost everyone would know someone who died.
“For the funeral industry, the great challenge will be the number of bodies that are likely to occur in a short space of time,” says Dr. Martin Meltzer.
There would be shortages of things like coffins and headstones. Experts say people who handle the dead would also be getting sick— everyone from funeral directors to grave diggers.
Health departments would set up temporary morgues. And as in 1918, there might even be mass graves.
“We collectively have to set new standards of decency to be willing to say, I want to treat my family member with dignity. But I know that there are a whole lot of other people just like them, wanting to do the very same thing,” Dr. Monica Schoch-Spana.
Day 120. The question would be, how much more can people take?
“How resilient are our communities? How long can people hunker down and stay home? How do we support critical infrastructure in the face of what’s likely large-scale absenteeism?” asks Dr. Martin Cetron.
The philosopher Nietzche once said, “What doesn’t kill us makes us stronger.” Those words would ring true as the nation and the world started to turn the corner.
Most people who get sick, would survive, and would be crucial to our recovery.
“Now these recoverers are going to be very special people,” says Dr. David Nabarro, UN Coordinator for Human and Avian Influenza. “They’re gonna have the immunity against the pandemic virus. They will be able to work in the hospitals.”
“We need them to help out. We need them to help out with their neighbors, with their friends, with their relatives, who may be sick down the hall. Help get them some food,” says Dr. Isaac Weisfuse, Department Commissioner for NYC Dept. of Health.
Day 150. The death rate would now be starting to decline, in part because of the immunity people have built. And chances are, as the virus circles the globe, it would continue to mutate — into a less dangerous form.
“It’s sort of the nature of evolution that for the virus to survive, it can’t kill off so many of its victims, or else it’ll just burn out,” explains Dr. Eric Toner, of the Center for Biosecurity.
And eventually that pandemic virus will then become the normal flu.
Day 180. The vaccine scientists have been developing for the past six months would now be available. But there still would not be enough for everyone.
So the question would be: who gets it first?
Health care workers would probably be among the first in line— along with police officers, firefighters, military personnel, and some political leaders. But the vaccine shortage would raise a moral dilemma over who should get vaccinated and who should not.
“Can you imagine the political consequences and the problems that are there with people dying lets say in Latin America, in Africa, begging for vaccine and we’re saying, ‘We don’t have any vaccine to spare?’” asks D.A. Henderson.
And now grim totals could be determined: Though experts say up to 40 percent of the world’s population could become infected with the pandemic virus, past pandemics indicate that only a small percentage would die. Still, the numbers of dead would be staggering.
“Worldwide, we could see 'as few deaths,' if that’s the correct term, of 7 million excess deaths. And all the way up to 100 million or even more,” says Martin Meltzer, Sr. Health Economist, Office of Surveillance, National Center for Infectious Diseases, CDC. “It is absolutely frightening.”
In the United States the numbers would be just as frightening. The Department of Health and Human Services estimates that in a severe pandemic, up to 90 million Americans — almost one third of the population — would get sick. Half of those 45 million would need medical care.
And almost 2 million people in the United States could die.
Day 365. The pandemic is over in most of the country, and the world. In our scenario, the stock market is beginning to recover after a steep drop, but thousands of workers who’ve lost their jobs during the pandemic are now looking for work.
Many hospitals would be financially devastated and near bankruptcy.
“Hospitals will lose money on every single one of those flu patients. So every hospital will be facing huge financial losses,” says Dr. Toner.
And it wouldn’t be just hospitals. Airlines, restaurants, tourist attractions would all be struggling to make up for lost business.
“And when the pandemic is over, and the realize their financial situation’s again stabilized their jobs are okay, they’re working again. And they need a new car, they are quite likely to go back down to the dealership and purchase it. So it will be a gentle recovery,” says Dr. Martin Meltzer.
Life would go on. Just as it has after past pandemics.
“The majority of us are going to survive. The majority of us are going to be around to tell the before and after story about when pandemic flu hit,” says medical anthropologist Monica Schoch-Spana.
But is everything that unfolded in this scenario inevitable? The shortages of supplies? Vaccines? The number of deaths?
Not necessarily.
The scenario we’re just shown you is based on a pandemic that would occur within the next few years. But if there is more time, there is more hope.
“We are pre-event right now. So, if we want to be able to say we acted decently in our neighborhood and our community and in our nation, we could actually take steps right now to do something about it,” says Dr. Schoch-Spana.
We’ve shown you what might happen if a pandemic were to occur soon. But does it have to be that way? Could a vaccine be produced sooner?
Could hospitals be better prepared?
We spoke to the Secretary of Health and Human Services, Mike Leavitt, the man charged with preparing the U.S. for the next pandemic.
Secretary Leavitt showed me the Command Center at the Health and Human Services Headquarters in Washington, DC.
Sec. Mike Leavitt: This we use this far more than we wish we did. This is where we’re tracking flu, it’s where we’re tracking storms, it’s where we’re tracking anything that could have an adverse effect on the people of United States, or our humanitarian interests around the world.
These days, Secretary Leavitt and his team have been watching as the avian flu— the H5N1 virus— spreads around the world.
Sec. Mike Leavitt: We’re watching the virus, literally, everyday. We know its mutating. All viruses do.
Like everyone we spoke to for this program, Secretary Leavitt says he hopes the virus never mutates to a form that can pass easily from human to human, causing a pandemic like the one we depicted in our scenario.
But the secretary is unsure anyone is ready as they could be.
Sec. Mike Leavitt: No one in the world is prepared for a pandemic. The nature of the event is unlike any natural disaster that humans deal with otherwise. We’ve been going through Katrina and analyzing what we learn from Katrina. Katrina was three or four hellish days and then on to recovery. A pandemic is a year or a year and a half...
Secretary Leavitt has been barn-storming the country, speaking to state and local health officials preaching preparedness. He argues it’s up to local governments to get ready.
Sec. Mike Leavitt: Any community that fails to prepare with the expectation that the federal government will be able to come in, rescue them at the last moment, will be sadly disappointed. Not because the federal government isn’t prepared. It’s because when it’s occurring in 5,000 communities at the same time, it’s local preparedness that will ultimately spell the difference.
Ann Curry, Dateline correspondent: President Bush asked for more than 7 billion dollars for pandemic preparedness. So far, Congress has authorized $3.8 billion—half of what he requested. $250 million of that is earmarked for State and local governments to prepare for a pandemic.
And to those people who say, our local and state governments, just simply cannot afford to prepare us, to protect us.” You say what?
Sec. Mike Leavitt: I say there are many things that your national government will be doing: developing vaccines, helping to develop stock piles, protecting our borders, monitoring the disease outside the country and inside the country. Those are things the federal government can do.
Curry: How long is it going to take before we in the United States feels ready?
Sec. Mike Leavitt: It will take three to five years for us to develop the manufacturing capability to produce the 300 million courses of a vaccine necessary to treat the entire American public.
President Bush’s plan does call for billions of dollars to streamline and increase vaccine production.
And the Bush plan calls for a national stockpile of the anti-viral Tamiflu—which may or may not help in a pandemic.
The U.S. is now in a long line with other countries to get an adequate supply from the one Swiss manufacturer. If a pandemic happens soon, officials say we won’t have enough.
Curry: Do you wish the United States government had made this a priority sooner?
Sec. Mike Leavitt: It would it have been better if we had started two years ago? Of course it would. Looking back is of no consequence at this moment. Looking forward is what we have to do.
In a world threatened by the possibility of a flu pandemic, what can we do now to protect ourselves and our families?
Some communities and many individuals are already taking action.
Health and Human Services Secretary Mike Leavitt has thought about what he and his family would do during a pandemic.
Ann Curry, Dateline correspondent: Among the most vulnerable are children. You have five of them. What are you going to do?
Sec. Mike Leavitt: Well I’m going to do what every parent will do during that period. I’m going to do all I can to protect them. It’s quite possible that I’ll keep them home from school during a period of time. I hope that my children will find themselves in an atmosphere where they have food and water that has been sorted and prepared for just such an occasion.
Secretary Leavitt and his team have come up with a Pandemic Flu checklist that would prove useful in any emergency. It recommends that American store a supply of water and non-perishable food that could last a couple of weeks. Include any medicine—especially vitamins or prescription medications your family might need.
Make sure you have a flashlight, batteries, and a portable radio, as well as tissues, toilet paper and diapers if needed. Keep a supply of extra cash on hand.
And come up with a plan for how your family could ride out a pandemic at home.
Dr. Peter Duchin, Chief of Communicable Disease for Seattle-King County talks about his family is preparing. “We’ve talked about the need to home school our kids if school’s closed. We’ve talked about how we would work from home and how I can get my work done while minimizing my interactions with other people and the public.”
Seattle, where Dr. Duchin works, is considered one of the best prepared cities in the nation. Officials there have already begun a public health education campaign.
“In the case of a worst case scenario, no matter how you look at it it’s ugly and the healthcare system is going to be overwhelmed,” says Dr. Duchin.
His goal is to inform people now, so they would be prepared— an enormous challenge.
Secretary Mike Leavitt, the man in charge of preparing America, is hoping for more time, and is dreading the call that tells him a pandemic has begun.
Sec. Mike Leavitt: If that call comes, we’ll do all that’s possible to assure that the lives of Americans are protected. But there’s no doubt if a pandemic occurs that people will become sick. Some will die. But our nation will continue. And we’ll find a way to become stronger and prosperous as people.
