At half-past midnight, the helicopters dropped off the wounded — fleeting silhouettes wheeled away on gurneys in the glow of blue landing lights, four soldiers among the last of thousands to pass through the “M.A.S.H.” of the Iraq war.
The makeshift sprawl of tents that received them, the Air Force Theater Hospital, Iraq’s premier trauma center and a war-zone fixture, will soon give way to a modern, “hard-sided” complex across the road.
The opening of that 107,000-square-foot hospital, in stages throughout July, not only brings a more standard, state-of-the-art facility to Iraq. It also announces that the U.S. military, after more than 3,500 dead and 25,000 wounded in four years of war, will be well prepared to deal with severe casualties for years more to come.
At a time when no target date has been set for a U.S. military withdrawal from Iraq, the new Balad hospital looks ready for an extended U.S. stay.
“It’ll be good for 10 years, depending on how well you take care of it,” said Col. Brian Masterson, the hospital commander.
Heat, tents, sandstorms
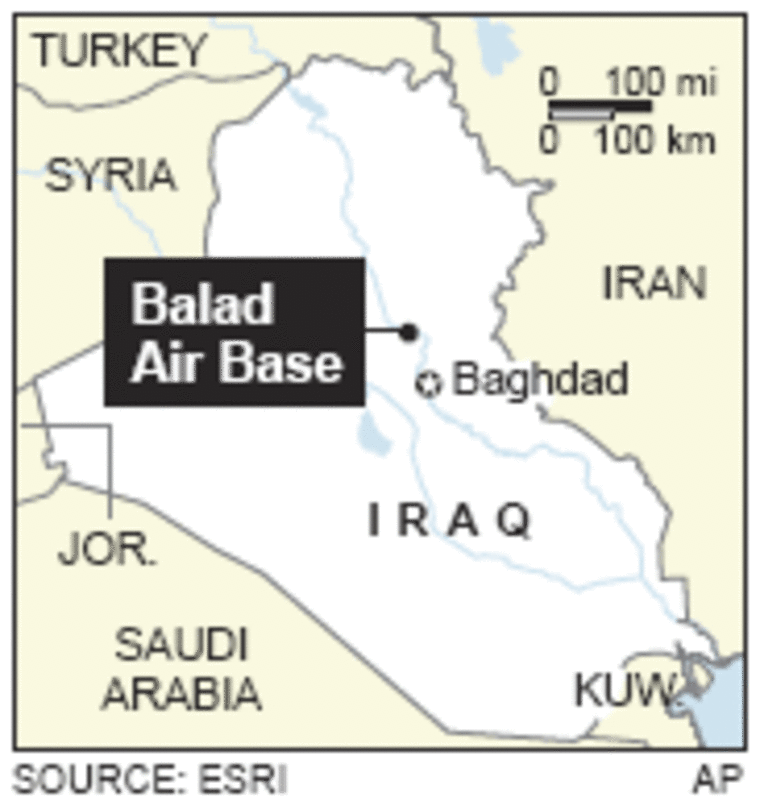
The staff in the existing “soft-sided” maze of tent flaps and wooden floors, covering 62,000 square feet at this base 50 miles north of Baghdad, say the care already ranks with the best.
“Don’t let our surroundings fool you,” said Tech. Sgt. Ellwood Tegtmeier, 35, of Pittsburgh. “We are state of the art. Except we do it in the heat, in tents, in sandstorms.”
The surroundings may evoke the Korean War’s Mobile Army Surgical Hospital, the M.A.S.H. of Hollywood and television fame.
But Balad’s 50 or so dun-colored tent sections house the most up-to-date equipment — the “16-slice” CAT scanner overseen by Tegtmeier, for example — and a broad range of expertise, from thoracic and vascular surgeons to the U.S. military’s only neurosurgeons in Iraq.
As the hospital grew and the tents spread year by year, the mayhem and tragedy of Iraq was funneled into Balad’s emergency room in sometimes daunting numbers. It once handled 35 casualties in a single 40-minute period.
The No. 1 mission of the hospital’s 379-member staff, largely Air Force regular and reserve personnel but also including Army doctors and nurses, is to perform emergency surgery and other procedures for troops badly wounded by blasts, shrapnel, bullets and burns, and prepare them for evacuation on nightly flights to the U.S. military’s Landstuhl Regional Medical Center in Germany.
From there, most of these seriously wounded men and women go on to military hospitals in the United States for longer-term care.
'Good to be here'
But Balad’s casualties are not just American. Among the side-by-side tents that serve as hospital wards, the Iraqi patient population at times has rivaled the American.
On one recent night, as the quiet was broken occasionally by moans, seven children lay in a 10-bed Iraqi ward, victims of explosions and other violence whose origins — crossfire, terrorism, U.S. airstrikes — usually remain murky to those who treat them.
Other wounded Iraqis — suspected insurgents — are often dropped off by comrades at the Balad base’s gates, to be picked up on routine runs by a hospital ambulance.
On this night, nurses and doctors crowded around the bed of an Iraqi newly emerged from surgery for multiple wounds. At the foot of the bed, among the medical staff in their scrubs, stood a soldier with an assault rifle — a guard watching over this captive, blindfolded insurgent.
“In the emergency room, we don’t actually know if it’s an American or an Iraqi, whether it’s a POW. It wouldn’t make any difference,” said Air Force Capt. Matthew Sena, 37, a Sacramento, Calif., surgeon and reservist taking a break on a busy night.
The concentrated wartime experience of repairing large numbers of damaged bodies can have a professional and humanitarian attraction.
“It’s a lot busier at times than it would be at home. It’s good to be here,” said Sena, who said he may extend his four-month duty tour.
“A typical city trauma center might admit 2,000 patients a year. We average 8,000,” Masterson said. And those numbers have grown.
High survival rate
Compared with the first four months of 2006, the hospital evacuated 25 percent more patients in the same period this year, Masterson said. That coincided with a rise in U.S. troop numbers and U.S. casualties in a new anti-insurgent offensive.
Masterson and his staff are proud of the 98 percent survival rate for the wounded that come through their emergency-room tent.
“This hospital rivals any trauma center back home as far as specialties,” the colonel said.
But doctors, nurses, technicians and others were looking forward to the move into the spacious new facility, which will offer 18 emergency-room beds, for example, triple the current number.
The new hospital — four steel-walled, interconnected buildings erected at a cost of $9.7 million — should also end problems with electrical power too erratic for some sophisticated equipment, with feeble air conditioning that allowed afternoon temperatures to top 100 degrees inside the tents, and with water supplies sometimes insufficient for intensive treatment of burns.
The U.S. command had vetoed a proposal for a $43 million “brick-and-mortar” hospital to replace the tents, to avoid giving the U.S. military presence too permanent a look, Masterson said. The new facility also wasn’t designed for eventual handover to Iraq’s health care system, he said.
