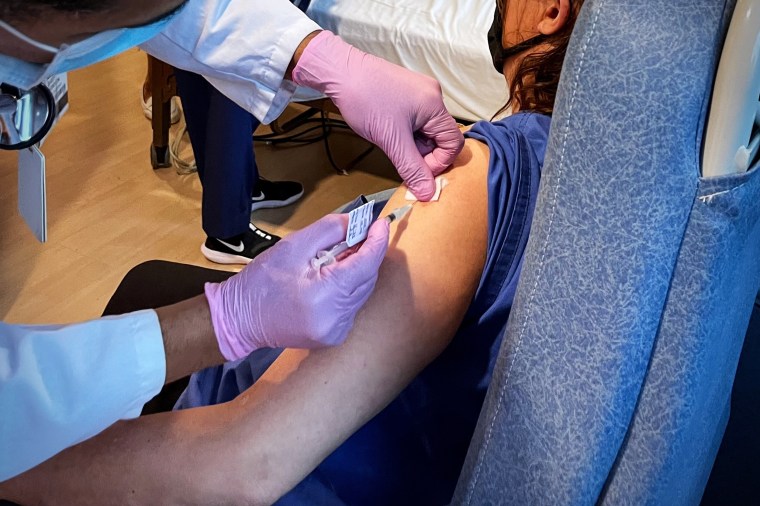
The vaccination felt like most others — a slight pinprick in M.'s upper arm, followed by the application of a Band-Aid and advice to monitor the injection site for any unusual reactions.
The vaccine, however, is unlike any other. It's not meant to protect against the coronavirus, or any germ, for that matter.
It is meant to protect against a deadly opioid overdose.
When M. (who requested that her full name not be used to protect her identity) got the shot this Tuesday, she became just the sixth person to receive it.
"It's very powerful now that I think about it," she said of participating in the trial, just a few hours after getting the vaccine.
The trial — the first to test the safety and potential effectiveness of an opioid vaccine in humans — is being led by Sandra Comer, a professor of neurobiology in the department of psychiatry at Columbia University's Vagelos College of Physicians and Surgeons, and Marco Pravetoni, of the University of Minnesota Medical School.
All of the participants, including M., are in active phases of addiction and are being housed at Columbia or another clinic for 10 weeks during the study. That's because researchers must give the participants nonlethal doses of opioids, including heroin, after the experimental vaccine to see how it works.
"These are people who are ongoing opioid users," Comer said. "We don't want to give that to somebody who is currently stable and doing well in treatment, because it might trigger a relapse."
If it ultimately proves to be effective, an opioid vaccine would be an "important and lifesaving option," said Dr. Nora Volkow, director of the National Institute on Drug Abuse. "We need as many effective tools as possible to accelerate our ability to prevent and treat opioid use disorder and overdose."
"The principle is pretty simple," Pravetoni said. It "triggers the patient's own immune system to develop antibodies against the target."
It's the same basic idea behind all vaccines: teach the immune system to make antibodies that will target and destroy a specific invader. Covid-19 vaccines, for example, work by training a person's immune system to identify and make antibodies that target the coronavirus’s infamous spike protein.
In the Columbia trial, the vaccine is targeting a specific type of narcotic: oxycodone, an opioid used in painkillers like OxyContin.
The vaccine would not prevent cravings for the drug — it would likely be used in conjunction with medications that do — but it could serve as an added layer of protection for people at high risk, Comer said. If they end up using oxycodone, the antibodies should bind to it and prevent it from getting to the brain.
That is key in reducing overdose deaths. Opioids kill by entering the brain, triggering a person's body to slow breathing down to dangerous levels.
While any clinical use of an opioid vaccine is still years off, the idea that a vaccine could stem the soaring opioid epidemic is gaining traction.
"There are a lot of people who are working on vaccine-type products for treatment" of opioid use disorder, said Sharon Walsh, director of the Center on Drug and Alcohol Research at the University of Kentucky, calling the work "inventive."
The approach "is one that, A, we think might last longer than other treatments, and, B, could be used in combination with them, which is even better," Comer said.
'The numbers are chilling'
Drug overdoses killed a record 93,331 people in the U.S. last year alone. Opioids accounted for about 70 percent of such deaths.
In 2019 — the latest year for which data is available — the National Survey on Drug Use and Health found that 1.6 million people were reported to have an opioid use disorder, meaning a physical dependence to opioids that's nearly impossible to quit, even with help from professionals.
"The vast majority of people who are dying of opioid overdoses were not people who just said, 'Hey, shooting up fentanyl seems like a fun way to spend a Friday,'" said Dr. Andrew Kolodny, medical director of the Opioid Policy Research Collaborative at Brandeis University in Massachusetts.
"If you're addicted to prescription opioids, you're not doing it because it's fun. You're doing it because you have to once you're hooked," he said.
It's not uncommon for people to be introduced to opioids through prescription painkillers, and go on to develop a dependency on stronger drugs, like heroin.
That is what happened to M., the Columbia trial participant.
She felt her addiction take hold the moment a doctor gave her Vicodin, an opioid painkiller, to help ease a toothache. The high was immediate and euphoric. M., who is in her forties, was left in constant search of the next high.
Within four years, M.'s addiction was so out of control, she was shooting heroin hourly. The magnitude of her illness is devastating to her.
I never grew up wanting to be a heroin addict.
"I never grew up wanting to be a heroin addict," she said.
There are potentially millions of others at risk. According to the National Institute on Drug Abuse survey, more than 10 million people reported misusing opioids within the past year.
"The numbers are chilling," Volkow said. The Covid-19 pandemic made a terrible situation with opioids even worse, she said, because "hospitals were not prioritizing treatment of substance use disorder."
What's more, Volkow said that people who needed treatment for their drug addictions were not seeking help at doctors' offices because they were afraid of the coronavirus.
Data from the Centers for Disease Control and Prevention found that the number of overdose deaths increased by nearly a third in 2020, compared with 2019.
The synthetic opioid, fentanyl — and its derivatives — has proven to be one of the biggest drivers of such deaths, the research found.
Fentanyl can be 100 times more powerful than morphine, and is often added to illicit drugs like cocaine and other drugs purchased on the street.
The fentanyl target
That opioid is the target of another vaccine in the works, developed by Dr. Ofer Levy, director of the Precision Vaccines Program at Boston Children's Hospital.
The research is still in its early stages, not yet out of animal and lab studies. In theory, the shot would work in the same way as the one being tested at Columbia, but target fentanyl instead of oxycodone.
Levy said anyone at risk for a fentanyl overdose could be a candidate for such a vaccine. "That includes those with opioid use disorder and potentially others who are at risk of taking a different drug that may have been mixed with fentanyl," he said.
This includes teenagers who, while they may not have a diagnosis of opioid use disorder, are at high risk of using street drugs that could be laced with fentanyl.

Katrina Hewitt, 41, of Attleboro Falls, Massachusetts, witnessed such a situation late last summer. A friend of her teenage son's had come to the Hewitt house after taking what she thought was the anti-anxiety drug, Xanax, purchased on the street.
In fact, it was laced with fentanyl and sent the friend into an overdose. Hewitt was able to save the teen's life with naloxone, an emergency medication to reverse an overdose.
Ideally, a fentanyl vaccine would be given to a person such as this — someone at risk for overdose, Levy said.
If that vaccinated individual were to then take a drug laced with fentanyl, Levy said the person's antibodies would "sponge up" those fentanyl molecules before they ever cross the blood-brain barrier. In theory, this would prevent overdose death.
Hewitt had previously been addicted to pain pills after they were prescribed to help her recover from several surgeries.
She is sober now and participates in the fentanyl vaccine research at Boston Children's.
Some participants in the study regularly give blood samples so the research group can test which vaccine candidates may work best in people with a history of opioid abuse.
Levy and his colleagues hope to move their vaccine into human safety trials within the next few years.
Other avenues of exploration
Walsh, of the University of Kentucky, said the challenge of any opioid vaccine research is to make that inoculation recognize a variety of opioids. "Heroin doesn't look like fentanyl, and fentanyl doesn't look like oxycodone," she said.
Indeed, both teams ultimately hope to create a so-called multivalent vaccine that would target multiple risky opioids. Carfentanil, for example, is 100 times as strong as fentanyl and 10,000 times more potent than morphine, according to the National Institute on Drug Abuse.
Researchers at Scripps Research in La Jolla, California, investigated a potential vaccine that could target both fentanyl and carfentanil. Preliminary data was published in the journal ACS Chemical Biology earlier this year.
The research, which is ongoing, was found to increase antibodies to both opioids in lab mice, and cut down on the amount of drug that reached the brain.
Kim Janda, professor of chemistry and immunology at Scripps who led the research, said his team is also focused on a different kind of overdose deterrent: a monoclonal antibody.
While vaccines prompt the body to make its own antibodies, it can take several weeks or even months to build a robust response.
An infusion or injection of a monoclonal antibody could be considered a bridge to a vaccine, Janda said, providing immediate protection in an emergency situation.
While emergency naloxone also acts quickly, the effects tend to wear off soon after, within a day or so. Janda suggested that an emergency shot of a monoclonal antibody may offer longer-lasting protection, at least for a few months.
A multipronged approach
Even if the vaccine is ultimately successful, experts say the shots will likely be paired with other addiction medications and counseling programs.
The multipronged approach reflects the magnitude of the opioid epidemic, Janda said. "You have to attack the problem from different directions."
Medications used to treat opioid use disorder, such as buprenorphine and methadone, work to cut cravings. They are effective, reducing the risk of overdose death by about 50 percent, said Walsh, of the University of Kentucky.
But she said, "less than 10 percent of people who need them can get access." To get a daily dose of methadone, Walsh said, people often need to go to a clinic seven days a week. That can be difficult for people who work and are raising families. Many may not have regular access to a vehicle.
This makes it "incredibly hard for people to stay in care," Walsh said. In theory, lasting antibodies from an opioid vaccine could help fill gaps in treatment.
What's more, Comer said that relapse occurs in about half of patients on such medications after about six months of care.
An opioid vaccine could help protect these patients.
"If after six months, a vaccinated patient relapses to opioid use, they would still have the antibodies circulating in their system," Comer said.
"It may provide protection from overdose, and allow us a window of time to re-engage them in treatment," she said.
But as opioid overdoses continue to rise nationally, it is clear that standard treatments do not always work as intended.
Buprenorphine, for example, did not help M. Neither did eight different stays at inpatient rehabilitation facilities.
"I would walk out the door and just pick up" using again, she said.
Still, she remains hopeful the vaccine will finally help her, as well as so many others struggling with addiction.
"If it can help somebody, or make a difference, that would be incredible," M. said. "That's what's pushing me forward."
Follow NBC HEALTH on Twitter & Facebook.
CORRECTION: (March 8, 2024, 11:27 a.m. ET): An earlier version of this article misstated Katrina Hewitt’s involvement in Boston Children’s opioid vaccine research. Other participants give blood samples; Hewitt did not.