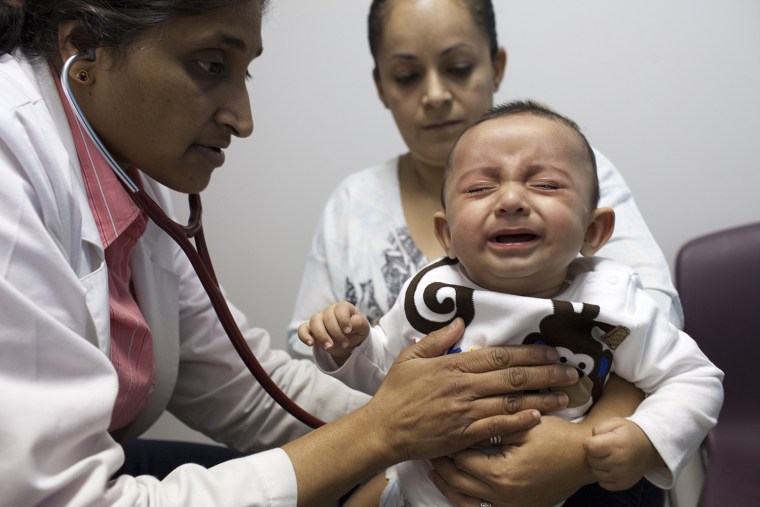
Midwives, nurse practitioners, physician assistants and other non-doctors do as good a job as MDs in the care they deliver — and patients often like them better, a World Health Organization team reported on Thursday.
These non-physicians are especially effective in delivering babies, taking care of people infected with the AIDS virus, and helping people care for chronic diseases such as diabetes and high blood pressure, the team reported in a WHO bulletin.
The findings extend from the poorest nations to the United States and Europe, they said. While some physician groups have resisted wider use of such professionals, they should embrace them because they are often less expensive to deploy and are far more willing to work in rural areas, the WHO experts said.
“There are some obvious advantages in terms of relying on mid-level health workers,” WHO’s Giorgio Cometto told NBC news in a telephone interview.
“They take less time to be trained. Typically, they cost less to remunerate. In some countries they are more likely to be retained in rural areas.”
David Auerbach, a researcher at the Rand Corp., says other studies have shown the same thing. “There’s really not much difference you can find in the quality,” he said.
Doctors are scarce in the United States. The Association of American Medical Colleges projects a shortfall of 90,000 physicians by 2020. Family practitioners and other generalists are especially scarce, and experts predict it will only get worse as millions of Americans get health insurance under the 2010 Affordable Care Act.
Doctors are also scarce in the developing world, and many countries are looking for ways to fill gaps.
Cometto and colleagues around the world looked at all the studies they could find on the quality of care delivered by non-physicians. They settled on 53 that looked specifically at the quality of care delivered — and at how happy patients were with the care they got.
“The evidence shows there aren’t statistically significant differences,” Cometto said. “The quality of care they provide is comparable to physicians. In some cases, for specific services, they actually outperform physicians.”
For instance, nurse-midwives or midwives who deliver babies end up using fewer drugs and they are less likely than doctors to make a type of cut called an episiotomy. Groups such as the American College of Obstetricians and Gynecologists recommend against episiotomies because they don’t heal as well as the natural tears that occur during childbirth.
Midwives were no more or less likely than doctors to induce labor, perform cesarean sections or use instruments to deliver a baby, Cometto’s team found, and the rates of death of either mother or child were the same among doctors as among midwives.
There were similar findings for treating patients infected with the human immunodeficiency virus (HIV) that causes AIDS. “One study compared the effects of antiretroviral therapy (ART) in patients managed by nurses and those managed by doctors. There was no significant difference in the likelihood of ART failure between groups of patients managed by nurses and those managed by doctors,” the researchers wrote. “Nor was there any difference in mortality, failure of viral suppression or immune recovery between the groups.”
When it came to caring for heart disease and diabetes, patients actually seemed to like nurses and other non-doctors better, the report found. This jibes with what nurse-practitioners and physician assistants working in the United States report. “We look at patients in a more holistic manner,” Judy Honig, associate dean at the Columbia University School of Nursing, said in a recent interview.
The Institute of Medicine, which advises the federal government on health matters, says nurses can do more than they already do and can help meet ballooning demands as the population ages and as more people get health insurance and start seeking care.
The United States has more than three million nurses. They already deliver much of the front line health care that Americans need, from giving vaccinations to delivering babies.
Nurse-practitioners are registered nurses who hold graduate degrees and can perform virtually all of the functions of front-line family doctors — depending on the laws of the state they’re in.
Between 1998 and 2010, the number of Medicare patients treated by NPs increased 15-fold to more than 450,000 people, University of Texas Medical Branch researchers found recently. Groups such as the American Association of Nurse Practitioners are calling for even more to be trained.
Physician assistants are also seen as offering a big plug in the health care hole “Currently, there are more than 93,000 PAs throughout the U.S. whose education in general medicine prepares them to be extremely nimble, positioning them very well to address an influx of 20 million new patients entering the health care system,” says Lawrence Herman, president of the American Academy of Physician Assistants.
Rand’s Auerbach says integrated clinics, using electronic health records and other technology, can really help fill the gaps. But he notes that not all medical groups are on board with the idea.
“It’s getting over a cultural barrier and learning how to work in teams of providers with different expertise,” Auerbach said. “That is not trivial.”
The American Society of Anesthesiologists recently spoke out against what it sees as the overuse of nurse-anesthetists. “Somehow there has become the notion that you can take physician extenders and replace physicians,” said Dr. Jane Fitch, a former nurse anesthetist who is now a physician anesthesiologist. “We are really concerned about patient safety.”