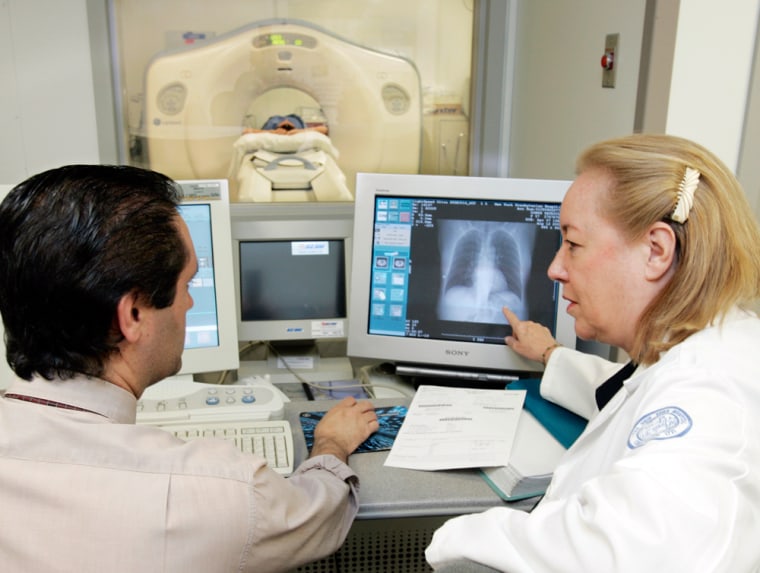
If a simple, painless test can find the world’s deadliest cancer when it is smaller than a pea — and such a test does indeed exist — shouldn’t people who are most at risk have one?
Surprisingly, the federal government, American Cancer Society and a raft of cancer specialists say the answer is “no.”
They are waging an uphill battle as frightened current and former smokers rush to get a special kind of X-ray that other physicians are urging for lung cancer detection but that has not yet conclusively been shown to save lives.
A huge federal study is under way to see if it can, and answers may come as soon as next year. In the meantime, it’s generating a classic “can’t wait for science” stampede.
The clamor rose last week with the deaths of newsman Peter Jennings and “Dallas” star Barbara Bel Geddes, and the news that “Superman” widow Dana Reeve has lung cancer.
Patricia Dowds and her husband, David Byrom, psychologists from Long Island, are among the many former smokers who voted with their wallets and had the $300 test on Friday.
“We do it for our own peace of mind,” Dowds explained.
No one disputes that the test, called a spiral or helical CT scan, detects lung abnormalities as small as 5 millimeters — less than a fifth of an inch.
The argument is over whether that’s a good thing.
For every cancer these scans detect, many more “false positives” occur — harmless bumps and lumps leading to painful, expensive and unnecessary biopsies and surgeries. Complications can include lung collapse, bleeding and infection.
“The concern that we have is false positive rates,” which range from 25 percent to as high as 60 percent, said Tom Glynn, the cancer society’s director of science and trends. “What we don’t want to do is create even more anxiety” by backing a test that is so imprecise, he said.
Early detection improves survival
Even when cancers are found, experts argue about whether that’s a benefit or a risk. No one knows how many of these tumors are so slow-growing that they pose less of a health threat than the surgery, radiation and chemotherapy used to treat them.
However, screening proponents say there’s no mystery about how deadly the disease is, and that survival improves the sooner it is detected. About 172,570 Americans will be diagnosed with lung cancer this year and almost as many, 163,510, will die of it.
The morning after Jennings’ death, the chairman of internal medicine at St. Louis University, Dr. D. Douglas Miller, contacted the public relations staff, urging them to get out the word on lung CT scans’ benefits.
Dr. Len Horovitz, a lung specialist at Lenox Hill Hospital in New York City, also has been urging the test. Though there’s no proof yet that it improves survival, “I can’t believe it wouldn’t,” he said. “There are half a dozen people I could bring into my office today who are alive for that reason.”
As for the risk of unnecessary followup procedures, “You don’t have to biopsy everything you see,” Horovitz notes. “You could also elect to watch it,” and do a biopsy only if the lump appears to be growing.
The scans’ biggest proponent is Dr. Claudia Henschke, director of the Lung Cancer Screening Program at New York-Presbyterian Hospital/Weill Cornell Medical Center, who published a landmark paper in 1999, reporting that the scans found far more lung tumors than conventional chest X-rays.
“We feel we have evidence that CT screening saves lives,” not just from that 1,000-person study but followup work on 30,000 patients around the world, she said.
But her study isn’t considered the gold-standard kind of evidence that insurers, policy-makers and scientists require. That will come from the huge randomized screening study the National Cancer Institute commissioned after Henschke’s paper appeared. The cancer society, the American College of Radiology and other professional groups are participating in the enormous effort.
As an indication of how eagerly anticipated this study is, doctors allowed themselves two years to recruit 50,000 people for it — and got 53,000, four months ahead of schedule, said Dr. Denise Aberle, the University of California at Los Angeles scientist leading the study. It will compare regular chest X-rays to CT scans and see whether either improves survival.
If it shows benefit, “I would feel great,” she said, but won’t recommend it until then, “and a lot of my peers and the scientific community are not.”
One is Mary Yagjian, coordinator of lung screening at the University of Pittsburgh Cancer Institute, who advised against testing for her own 82-year-old mother, a former smoker at high risk of lung cancer.
“She’s scared to death about getting it,” and has a brother just diagnosed with cancer and a friend going through a recurrence now, according to Yagjian.
“It’s important that we complete the definitive studies and get scientific information,” said Dr. Christine Berg, chief of the early detection research group at the cancer institute. In the meantime, doctors have to do the best they can to advise each patient, considering that person’s smoking history and other risk factors.
“It’s the physician-patient relationship that’s paramount,” she said.
As contentious as CT scans are, some people are seeking even more controversial tests — whole body scans. Two years ago, at the insistence of his wife who did not trust the clean bill of health he’d gotten from a regular chest X-ray, Hy Muroff of Windsor, Ontario, went to see Dr. Marc Kahn at EBT-Heart & Body Imaging in the Detroit suburb of Southfield, Mich.
Muroff, 78 at the time, had smoked but not for 20 years. The scan showed a tumor behind his heart; the growth was removed in surgery. He called to schedule another full-body scan a few weeks ago, after hearing that Jennings was diagnosed with lung cancer, to make sure his disease hadn’t recurred.
People should get such scans, Muroff said, “only if you want to stay alive.”