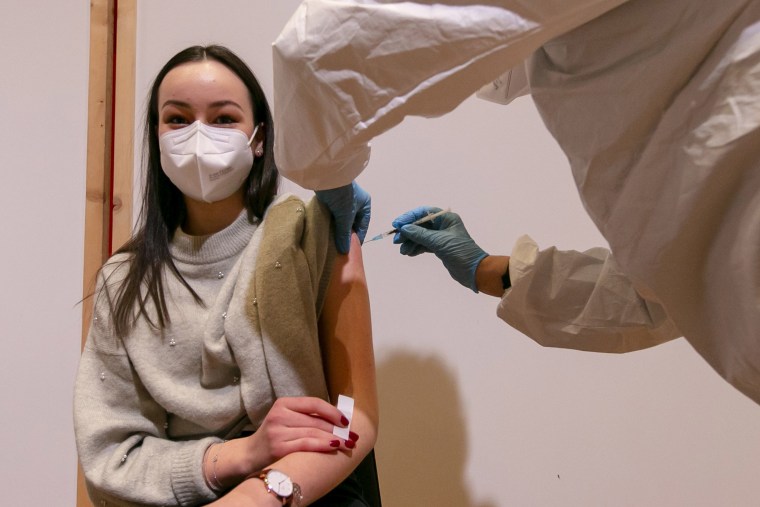
Hope is alive. Covid-19 case rates and hospitalizations are falling fast. The three available vaccines are remarkably effective. Soon most adults — and our adolescent kids — will have the chance to be vaccinated.
This is great news, particularly for us women who have uniquely suffered during the global pandemic. As primary caregivers, we’ve juggled work without the typical support of childcare and school. We’ve been losing jobs at a far higher rate than men. Additionally, many of us are taking care of our aging parents and the bulk of household duties.
As a result, it’s no surprise we are stressed.
Take my patient Colleen, a working mother of four, whose stepmother died unexpectedly during Covid-19. The stress of parenting combined with social isolation has made coping with loss even harder.
I am a primary care doctor, and I’ve found that of my patients are grappling with some degree of pandemic-related stress, anxiety, loss or grief. If you are anything like myself and my patients, your mental health affects your overall health and well-being.

As we approach re-entry, there’s also newer feelings of stress ― and even a fear of normalcy. So how do you get back into the driver’s seat of your own well-being? I invite you to examine these four chapters of your pandemic story, and consider the ways you might author it anew:
Sleep.
Sleep is essential for our health, but getting enough of it can be annoyingly elusive when stress takes over. Some of us simply don’t have enough time to get rest. Others have trouble winding down after a multitasking, coffee-fueled day.
The average adult needs seven to nine hours of sleep to help cope with stress and to boost mood, but fewer than two-thirds of women get it. I regularly advise patients to turn off all screens an hour before bedtime and create a bedtime routine to promote calm. Meditation apps like Headspace or Ten Percent Happier can help you get started. Limiting caffeine and other stimulants also helps cut the engine of sleeplessness and stress.
Eating.
Most of us know how to eat healthfully, yet it’s easy to gravitate toward comfort foods or skip meals when we’re on the run or feeling anxious.
Healthy eating is important for our bodies and brains; so is an awareness of our sometimes-complicated relationship with food. Women have unique nutritional needs. Eating protein, fiber, grains and healthy fats throughout the day is important; it’s equally essential to identify triggers for emotional eating. When we name underlying stressors and address them head on, it’s easier to fuel our bodies for the day ahead.
Moving.
Exercise is essential for our mental health, but it can be the first thing to go when we’re busy. With gyms closed and Zoom calls unending, it’s no wonder we’ve been generally more sedentary in the pandemic.
Yet moving is medicine! Physical activity tamps down our stress hormones, lessens anxiety and boosts mood. It doesn’t have to be fancy, formal, or fanatical; we simply need to move! Walking outdoors is a wonderful way to enjoy nature and movement and even to safely socialize. I commonly recommend yoga for posture, strength and mindfulness all in one.
Connecting with others.
Women are naturally gregarious creatures. Stripped of our social lives and in-person supports for over a year, women are starved for female companionship and fun. Connecting with friends and loved ones is part of how we cope.
Once you’ve been vaccinated, it’s time to practice reconnecting with others. Even before you’ve had the shot, it’s possible to socialize safely. So let’s get out there! It does a person good from the inside out.
Although I can’t take away the pain of Colleen’s unexpected loss, I could help her cope by encouraging her to socialize safely, eat regular meals, keep moving her body, and get the rest she needs.
We’re gradually winning the race against coronavirus, but we have a long road ahead. The first step is to recognize the relevance of your relationships with sleep, food, exercise — and even to your own body — to your mental health. Assessing them now, on the cusp of normalcy, will help us open the door to improved health and well-being.
Lucy McBride, M.D., is a practicing internist in Washington, D.C. A trusted and recognized voice in patient care, she is the author of a popular COVID-19 newsletter working to increase awareness of the intersection of mental and physical health. Sign up on her website and connect with her on Twitter, Facebook, Instagram and LinkedIn.