Growing up, Jenely Sarette’s Filipino-American family didn’t talk about sex education, and when they did talk about sex, it was more of a warning than anything else.
“In Asian-American families, including mine, sex isn’t talked about,” the 27-year-old Sarette told NBC News. “Rather, it’s more about instilling fear about sex. The only sex education I got from my family was: Don’t do it until you’re married. There was never really an openness about sexuality. It was a very uncomfortable topic.”
"We must continue working to develop culturally relevant strategies to break down myths, cultural barriers and stigmas around sexual healthcare among API women, their significant others, and their service providers."
In Yvonne Tran’s Chinese Vietnamese-American household, it was even worse. Her parents didn’t know the words nor did they have the tools to talk about sex.
“My mom didn’t have all the vocabulary to explain what sex education is to me, even if she wanted to,” the 30-year-old told NBC News.
These kinds of home attitudes have pushed some Asian-American women to seek their sex education on their own, whether through schools or outside organizations, where they may find culturally insensitive sources of information, according to research conducted by doctors at Boston University and the Center for Disease Control and Prevention (CDC). Those same attitudes can also lead to increased health risk, according to research from Boston University.
“I was able to ‘figure it out’ and go to Planned Parenthood, but not without a lot of confusion and shame at first,” 25-year-old Chinese American Jenny Dorsey told NBC News.
“My family was not open about sex, so my questions were mainly answered at school. I don’t know if that was a Catholic thing, or just that my parents were really poor communicators,” 37-year-old Sri Lankan-Lithuanian-American Sezin Koehler told NBC News.
While the topic of sex education is a challenging for families across the board, five Asian-American women that spoke to NBC News point out challenges of poor communication, and a cultural context of “shame,” “embarrassment,” and “fear” attached to sex. Many Asian cultures have different religious and cultural proclivities that affect their approach to this topic, making it challenging for first generation daughters to receive support, the women said.
"My mom didn’t have all the vocabulary to explain what sex education is to me, even if she wanted to."
In addition, some interviewees also mentioned not having enough providers who could talk to them about sex education and birth control from a culturally sensitive point of view, making the process even more uncomfortable.
“There are many Hmong families that have multiple children and there are many that just have one or two,” Hmong American Lyia Jalao, 26, told NBC News. “But there are not many family planning or reproductive health forms or workshops that are catered to the Southeast Asian community. I believe that this lack in reproductive health dialogue puts many Hmong girls and women in harm’s way.”
“My first encounter with reproductive health provider was at Planned Parenthood,” Tran said. “I remember the immense amount of shame I felt going there and thinking, ‘I’m one of those girls, I admitted that I had sex, and now I made a mistake by not using protection.’ I also felt like the provider kind of shamed me too. The way they talked to me, it sometimes feels like doctors assume I’m coming from a particular socio-cultural class with attached health issues, and they speak to me based on that profile.”
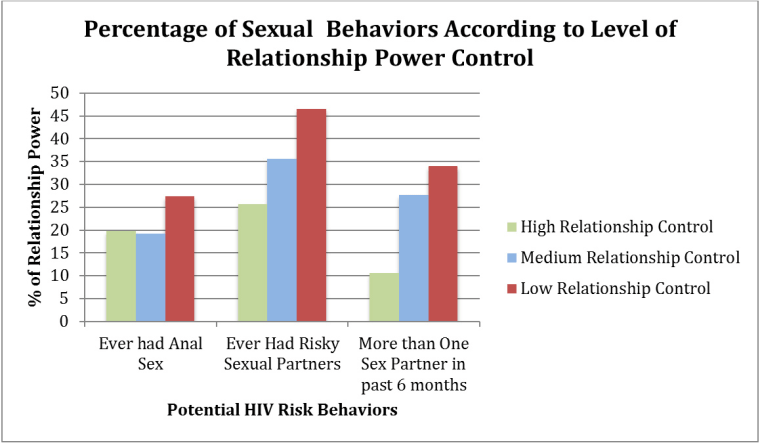
Those attitudes have been a detriment to Asian American’s sexual health.
According to a study done by Dr. William Adih and other colleagues published in the “Journal of the International Association of Physicians in AIDS Care,” the taboo surrounding sexual healthcare is correlated to the fact that “APIA women are emerging as a group vulnerable to STIs and HIV infection."
Professor Hyeouk Chris Hahm of Boston University has found in her research that other cultural factors also contribute to the trends. “This cultural expectation for women to be submissive and accommodating affects her ability to have discussions about HIV risk and consistent condom use," Hahm told NBC News. "In fact, APIA women who perceived to have lower relationship power were significantly more likely to be engaged in HIV related risk behaviors.”
“Furthermore, this stereotype of Asian-American women as a model minority group who are sexually conservative may also come into play in the disparity in access of APIA women to sexual health education," Hahm added. "In fact, APIA women in our study showed that they had similar level of HIV risks (forced sex, anal sex) compared to other US ethnic minority women."
Family Planning
Asian-American women also have different approaches to how and when they should start a family, often times conflicting with ideas of their parents’ generation.
According to research by the CDC, Asian-American women expect to have an average of 2.2 kids per family, tying with white women for the lowest expected birthrate. The median age for first birth is 26 years old, and Asian-American women have the lowest probability of having a birth by age 20, in comparison to other cultural groups.
“I believe I’m already overdue,” Dorsey said. “My mother had me at 24. My cousin had a baby at 24 too. But I prefer to have children around 30-35. I would like to be at a point in my career where I can take time off to enjoy pregnancy, focus on my children, and ease back into working without the stress of falling behind."
RELATED: Girls on Most Effective Birth Control Less Likely to Use Condoms
On the other side of spectrum, some women prefer to be child-free. “For me, being child-free is like taking the road less traveled, and the freedom is intoxicating,” Koehler said. “I think I always knew I didn’t want children. I considered getting a traditional, arranged marriage when I was younger, but when I found out the wife was expected to bear multiple children, I nipped the whole conversation in the bud.”
For those who do have children, other pressures arise. Sarette had her first child at age 21, and is now a single mother of two. Though her parents accept her choices, many Filipinos don’t understand the concept of co-parenting, she said. “When I go to the Philippines, they always ask about a husband," she said. "I feel pressure to get married. I feel like there’s shame in single parenting, which I think is rooted in strong Catholic beliefs. But I have gone against the expectations of ‘staying together for the kids’ and made a conscious choice to show my girls what they should accept in their life and what they shouldn’t.”
"In Asian-American families, including mine, sex isn’t talked about. Rather, it’s more about instilling fear about sex. The only sex education I got from my family was: Don’t do it until you’re married."
For women who are not dating men, family planning can be even more complex. “In queer relationships, you can’t just get unintentionally pregnant — you really have to talk about it and ask a lot of questions. Do we adopt? Do we want a surrogate? What race do you want them to be? The list goes on,” Tran, who identifies as queer, said.
As their choices in family planning reflect a Western upbringing, it can often create tension between generations.
“For a number of reasons my Sri Lankan father never really considered me Sri Lankan as he associated my independence, outspokenness, willfulness as American qualities, not those of a submissive Sri Lankan woman,” Koehler said.
RELATED: 'We Have to Please Ourselves First': Sex Talk With Margaret Cho
“Hmong girls are really pushed into pursuing higher education these days, but to do so while maintaining the ideal family life: have a degree, start a family, become the support system for their in-laws and husband's side of the family,” Lalao said. “Hmong girls are no longer pushed to have a family at 18 years and under, but the culture of shame around female sexuality still exists.”

Regardless of what approach Asian-American women choose to take with their family planning, there are solutions to help make it easier to access birth control. Dr. Sophia Yen co-founded Pandia Health, an automated birth control service scheduled to launch this summer. “One of the top three reasons women don't take their birth control is because they ran out," Yen told NBC News. "I co-founded Pandia Health to makes women's lives easier and prevent unplanned pregnancies by taking away the stress and hassle of having to worry about running out of your birth control every month.”
For those Asian-American women who are ready to pursue motherhood, Yen said the risk of fetal abnormalities goes up at 35, though new medical technologies may raise the threshold.
Additionally, she recommends that to optimize fertility levels, “Women should get tested for STIs annually if they are sexually active, and to get the HPV vaccine if they are 26 years old or under. She should also build a healthy body mass index and eat healthy. If a woman is overweight or obese, it will be harder to get pregnant. If periods are irregular, see your provider for testing. If you are trying to get pregnant, start taking prenatal vitamins,” Yen said.
As Asian-American women choose their own ways to approach reproductive health, birth control, and family planning in their lives, there is one thing that remains true. “We must continue working to develop culturally relevant strategies to break down myths, cultural barriers and stigmas around sexual healthcare among API women, their significant others, and their service providers,” Hahm said.
Follow NBC Asian America on Facebook, Twitter, Instagram, and Tumblr.