Dr. Sheryl Recinos’ patient refused to accept her diagnosis of Covid-19. Her cough was because of Recinos’ perfume, the patient insisted, certain that her positive Covid-19 test could not be correct.
Recinos, a family medicine hospitalist in California, was not wearing perfume. The test result, Recinos told her patient, was accurate.
The interaction, in summer 2020, was an outlier at the time. But in recent months, such conversations have become more common.
Recinos has treated people who, two weeks into hospital stays for Covid-related breathing struggles, still do not believe they have the coronavirus. She has had patients who have questioned her judgment, patients who have demanded to be given the same medications that former President Donald Trump received when he had Covid and family members of patients who have screamed at her for something as simple as giving their loved ones oxygen, a necessary treatment that they argue is doing more harm than good.
“It’s baffling. I’ve never seen anything like this,” said Recinos, who works 12-hour shifts for up to 20 days straight. “So many of us have worked so long and for so many hours, and we’re being undervalued by the general public.”

The fourth wave of the pandemic has brought unique challenges for front-line health care workers, many of whom were already nearing their breaking points.
Exhausted amid hospital staff shortages and emotionally depleted, health care workers also face growing skepticism and rage from patients, leaving workers frustrated and fearful.
“Our patients don’t trust us anymore,” said Amy Arlund, an intensive care unit nurse in Fresno, California. “A year and a half ago, the emotion that came with the influx of these patients was sympathy, empathy, remorse, guilt — and that well of emotion has dried up. What is left is anger and hostility and mistrust.”
The problem is on the rise across the country. In Missouri, one hospital is equipping its staff with panic buttons after assaults by patients tripled in the last year. In Idaho, family members who do not believe Covid is real have accused doctors and nurses of killing patients. And at a hospital in Massachusetts, at least two or three nurses are assaulted by patients every day, Boston NPR station WBUR reported.
In interviews, doctors and nurses alike said they feel defeated, by either the increase in animosity from patients or the refusal of many in their communities to accept that masks and vaccines are safe and effective ways to keep people from overwhelming hospitals in the first place.
All asked that the institutions that employ them and, in some cases, the cities they work in be omitted to protect their safety and because their views do not reflect those of their employers.
Dr. Mona Masood, a psychiatrist who is the founder and chief organizer of Physician Support Line, a confidential hotline she created for doctors at the start of the pandemic, said more physicians have been calling lately expressing that they have been the targets of vitriol.
“We’re calling it the ‘heroes to villains narrative,’” Masood said, adding that at the start of the pandemic, when health care workers were thanked with nightly displays of gratitude, doctors felt as though they were being celebrated as heroes but were worried that they did not have enough tools to live up to the expectation.
Now, she said, doctors call Physician Support Line feeling overwhelmed by how rudely they are being treated. Sometimes, she said, they will call quickly during their shifts.
“They call us and they’re like, ‘Let me get it out with you so I can get back in there, because heaven forbid I’m not the most professional I can be — people are going to blame me for that, too,’” she said. “They feel like they’re trapped.”
‘We have had very few breaks’
Staffing shortages in the medical profession predate the pandemic, but they have become particularly pronounced as hospitals have swelled with Covid patients.
“Everyone is in crisis mode all of the time,” Arlund said. “Your body is not meant to maintain that for 18 months straight.”
Up until last month, Arlund had been a crisis nurse, a specialty position that required her to tend to the ICU patients most at risk of deteriorating. In recent months, such patients have demanded treatments like ivermectin, a false cure for Covid; asked for medications she has never heard of in her two decades as a nurse; and generally expressed suspicion toward her and her colleagues.
In mid-September, Arlund had a Covid patient whose oxygen level was far below where it should have been. The patient was refusing to wear a specialized oxygen mask or agree to sleep on his stomach, a move to help him avoid going on a ventilator.
When Arlund and her co-workers ordered him to put on the oxygen mask, the patient — turning purple at that point— responded that Arlund was blocking his view of the football game on the television.

“I reached my point where I just had to walk away,” said Arlund, who has lost six colleagues to the coronavirus. She resigned as a crisis nurse while remaining a nurse in the ICU.
Attacks on those in the medical field are not limited to hospitals. Dr. Kellie Snooks, a pediatric ICU physician in Wisconsin, said pediatricians are coming under fire on social media for urging mask mandates in schools.
Snooks fervently stands behind mask mandates. As the highly contagious delta variant of the coronavirus has spread, her pediatric ICU has been filled to capacity, which rarely happened before the pandemic.
“People think health care workers have hidden agendas, and we don’t,” Snooks said, adding that she was bewildered that there is still opposition even with science proving that masks stop the spread of the virus and that vaccines are safe. “We just want people healthy, and we’re exhausting ourselves and stressing ourselves in the process of doing that.”
How to help ease the burden
Masood, the founder of Physician Support Line, said health care workers need more mental health support, starting with changes in the culture of medical school, where the residents who take the most shifts in a row are often the ones who get the most accolades.
If you or someone you know is in crisis, these resources can help
Her support line has received 3,000 calls since March 2020, and it is getting its highest volume of calls now. The 800 volunteer psychiatrists who answer the line give callers resources for more support if they need it at the end of the call or strategies such as mindfulness exercises.
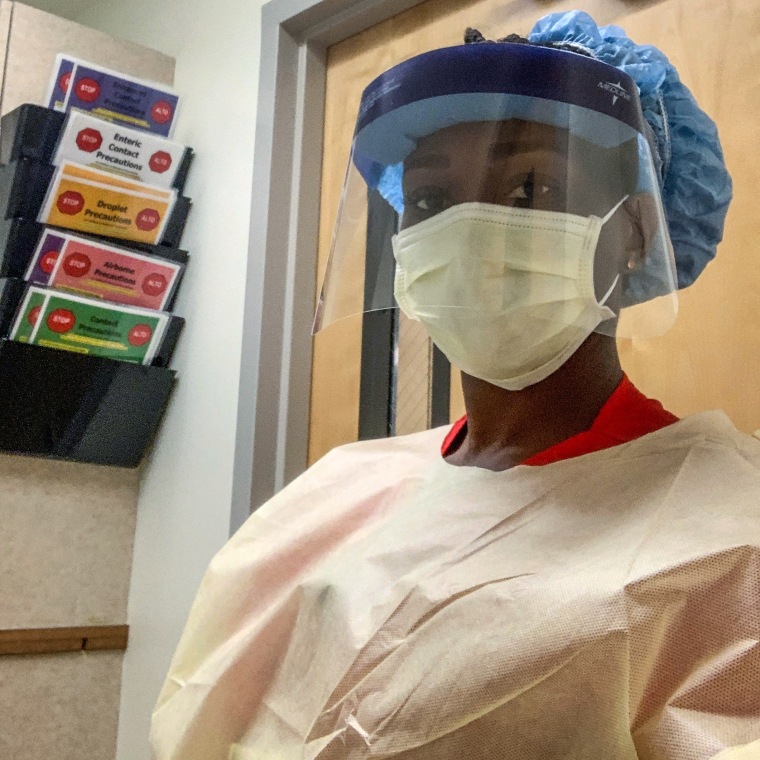
“We’re really trying our best to give the public the information that is necessary for them to protect themselves, but our words are only as powerful as how seriously they’re willing to take it.”
emergency room nurse MAWATA KAMARA
For Mawata Kamara, an emergency room nurse in California, taking mental health days off from work has been helpful. She has also started declining extra shifts, which she felt she could not do in the first and second surges of the pandemic.
“I’m not burning myself out again,” Kamara said.
She and the other health care workers interviewed for this article pleaded with people to vaccinate themselves and their families.
“We’re really trying our best to give the public the information that is necessary for them to protect themselves, but our words are only as powerful as how seriously they’re willing to take it,” Kamara said.
Others said they are asking people to do whatever they can to stay out of the hospital.
It is more than just getting vaccinated, wearing masks and practicing good hand hygiene, said Lindsey Harris, president of the Alabama State Nurses Association.
“How can we prevent those comorbidities — diabetes, heart disease, those things — where patients’ outcomes could possibly be better if they were to contract Covid?” she said.
Writing has always been an outlet for Recinos, the family medicine hospitalist, and it has helped her cope during the pandemic.
When the fourth wave started, Recinos could not bear to see as much loss as she saw last year. She temporarily transferred out of her home county, Los Angeles County, which has a low vaccination rate, to a hospital in a county with a much higher vaccination rate.
She still sees Covid patients, and the problem of misinformation is pervasive, she said.
“I have never admitted a patient for a reaction to the vaccine, but I’ve admitted so many patients for Covid,” she said. “I don’t understand why it had to become political.”
If you are a physician or a medical student in need of mental health support, call the Physician Support Line at 1-888-409-0141 from 8 a.m. to 1 a.m. ET, seven days a week. Calls are free and confidential. Other front-line health care workers and first responders can get free, confidential support from Magellan Health’s crisis text and phone line.
