JACKSON, Miss. — The children’s park near Lacy Lancaster’s home offers a clear view of the helipad at Ocean Springs Hospital, a few miles outside of Biloxi. Her two young daughters often plead to go to the playground, so they can watch flights touch down. Through their eyes, the sight is more awe-inducing than grim.
“There’s a helicopter coming to Mommy’s work and they want to see it land,” said Lancaster, a registered nurse in the hospital’s coronavirus intensive care unit.
There has been more helicopter traffic lately, as Covid-19 patients fill the Singing River Health System’s beds across its three campuses. More than a fourth of the network’s Covid patients are in critical care.
Lancaster has recently cared for several patients in their 20s and 30s; one, who has children, broke down in tears before she was put on a ventilator.
She is still fighting, but not all of Lancaster’s patients pull through. Her most difficult shifts, “when things don’t go right,” she said, are followed by emotional phone calls with a colleague.
“You’re crying,” she said. “You’re putting yourself down a lot. There’s a lot of anger. There’s a lot of sadness.”

Three hours north at the Children’s Hospital of Mississippi in Jackson, Rosie Barlow has spent days worrying over whether her son Donovan, 11, will wake up, each time he drifts off to sleep. Instead of dancing around the house and playing video games with his older brother, he is hospitalized and receiving breathing treatments. Donovan is among 28 patients confirmed or suspected to have the virus at the state’s only children’s hospital.
His parents say Donovan was weeks away from being vaccinated when he contracted the virus. He would have become eligible as soon as he turned 12 on Sept. 22.
“It’s a lot for our 11-year-old to go through, laying in bed and just wondering if, ‘I’m going to make it the next hour,’” Barlow said, though his condition began to improve this week.
This is what the fourth wave of the pandemic in Mississippi looks like: As of Thursday, only seven ICU beds were available in the state, and 96 patients needed them, according to the state Department of Health.
Nasal cannulas are brought out to waiting rooms to deliver urgently needed oxygen. Patients spill into hallways. Parents of children like Donovan try to remain strong as their child who was just attending school a week ago receives steroids and shots meant to prevent blood clots administered to his stomach. Nurses, like Lancaster, labor under layers of protective equipment as they struggle to turn heavily sedated patients facedown in hopes of expanding their lungs.
For weeks this spring, a steep drop in Covid cases and hospitalizations statewide seemed to defy Mississippi’s standing as one of the least-vaccinated states in the nation.
In July, the delta variant began reversing the relative lull in serious Covid cases. From July 18 to July 31, the statewide number of people with Covid in ICUs doubled, while the number in hospitals and on ventilators more than doubled. This month, the state set a new single-day record of Covid hospitalizations and patients placed in intensive care and on ventilators. Almost 90 percent of patients in hospitals with Covid from July 22 to Aug. 18 were unvaccinated, according to the state Department of Health.
Mississippi remains second to last in the nation for vaccination rates. Some in the state have spurned the vaccine due to political beliefs or misinformation. Others are concerned about their immigration status being exposed; the state Department of Health does not require IDs for vaccination, but the fallout from workplace immigration raids in 2019 have left many hesitant. Mississippi is also the second highest uninsured state in the nation, leaving many residents without access to primary care and a mistrust of the health care system.

The latest sign of the increasing strain on Mississippi’s hospital system came Wednesday, as state health officials announced that off-duty emergency medical technicians and certified paramedics would be allowed to provide aid to patients in the state’s hospitals. Hospital administrators across the state are scrambling to fill a nearly 1,500-person staffing shortage.
“We are clearly at the worst part of the pandemic that we’ve seen throughout, and it’s continuing to worsen,” Mississippi Health Officer Dr. Thomas Dobbs said.
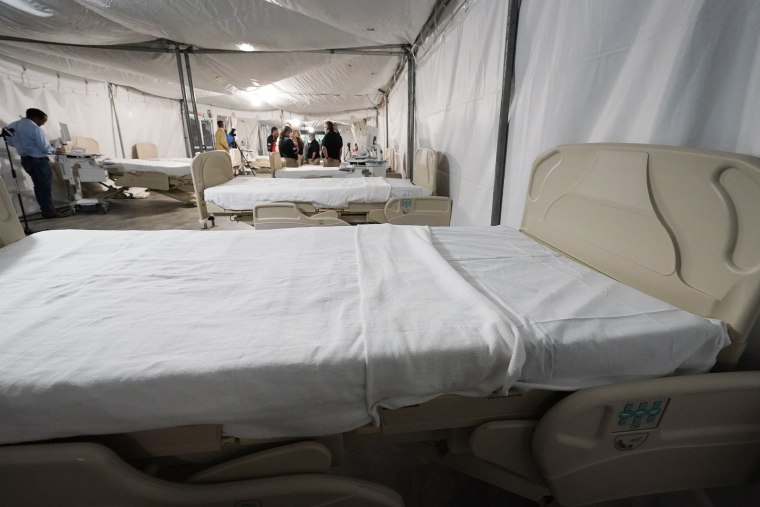
The University of Mississippi Medical Center, the state’s only Level I trauma center — a designation indicating that the medical campus is well staffed to handle life-threatening injuries — now has a temporary field hospital in its parking garage. A federal team is staffing the operation. Within days of the unit’s completion, a Christian charity organization, the Samaritan’s Purse, built a separate 32-bed facility on the campus, staffed by a team of 53 medical workers.
The virus shows few signs of abating among young people. Less than a month into the new school year, more than 20,000 students, or nearly 5 percent of children, in Mississippi’s public schools have been sent home to quarantine.
Gov. Tate Reeves, a Republican, has repudiated calls to reimplement a statewide mask mandate in public schools this year. Instead, local school boards and superintendents will decide whether to require coverings.
Dr. Anita Henderson, president of the Mississippi chapter of the American Academy of Pediatrics, said some districts with mask-optional policies have reversed course amid schoolwide outbreaks. But others waver on issuing mandates.
“There are some school districts and some school boards who are also saying things like, ‘We don’t know who to trust.’ They may hear from one group of doctors that say one thing; they may hear from other parents who are telling them something else,” she said. “By having a universal policy, direction from the governor’s office … I believe that all the school districts would be getting the correct information, the correct data and have the opportunity to listen to the voices who have the experience and the expertise.”
Bailey Martin, a spokeswoman for Reeves, said he does not plan to issue a mask mandate.
“He is allowing flexibility for the leaders of local districts — the ones who are uniquely positioned to understand the rapidly changing Covid-19 situation in their respective communities — to make those decisions,” Martin said in a statement.

While most children with Covid recover without becoming seriously ill, the bouts that end in complications can be devastating. Several patients at Mississippi Children’s are on ventilators. One death from Covid complications has already been reported this school year: Mkayla Robinson, an eighth grader attending public school in Smith County, died on Saturday. She tested positive for the virus the day before.
In rural Neshoba County, a hospital had to transfer a 2-year-old Covid patient to a pediatric hospital for care. Nearly half of Neshoba General’s 24 beds remain filled with Covid patients, including two in their 20s.
The community currently has the highest per-capita rate of new infections in the state, and the lowest vaccination rate, with 22 percent of the county’s population fully vaccinated. Cases surged following the Neshoba County Fair in late July, an annual event that brings visitors to campgrounds lined with neon-colored cabins strung with Christmas lights for political speeches, horse races and amusement rides.
Addressing fairgoers gathered on wooden benches under a pavilion on July 29, Reeves derided the Centers for Disease Control and Prevention’s revised guidance for vaccinated people to wear masks as “foolish.”
Dr. Andrew Dabbs, chief medical officer for Neshoba General, said the fair would not have pummeled the community if the state overall had a higher vaccination rate.
“I think the take-home message is if 90 percent of the people at the fair had been vaccinated, this would not be happening,” he said. “The real culprit is our low vaccination rate.”
Last week, he said, hospital staff members were encouraged when about a fourth of tests administered at its drive-thru testing site came back positive. The highest average was 41 percent.
“It’s very telling of our situation that we get excited that the number is down to 24 percent,” he said. “That kind of tells how bad this latest surge is.”

In recent days, the state’s public health leaders, as well as Reeves, have repeated the CDC’s warning that the crisis is now a “pandemic of the unvaccinated.”
“My personal sense is it’s 100 percent of the patients that I’m taking care of that are unvaccinated,” said Dr. Jawauna Stewart, a hospitalist in Hattiesburg.
One of her newer patients, a 23-year-old, told her she had planned to get vaccinated the next week — the virus had just caught her first.
As with other medical campuses, beds at Hattiesburg Clinic Hospital Care Service are scarce. Stewart has struggled to balance her time with patients during rounds. She visits her floor’s Covid ward first. Patients with the most severe cases are so ill, they are unsure what day it is. Trying to walk their families through treatment plans by phone is often discouraging.
“To be honest, that’s one of the most frustrating things because I rarely have good news,” she said.
A constant challenge is the looming sense that such outcomes are largely avoidable. A friend of Stewart’s, who works in a hospital in Texas, texted her when she lost two mothers who had become critically ill from the virus. Both women were in their 40s and unvaccinated.
“A little kid without parents, that’s heartbreaking,” Stewart said.
Hattiesburg is a college town, and campus leaders at The University of Southern Mississippi have rolled out a lottery for free fall tuition for students who show proof they have been vaccinated. Lucas Williams, the student body president, speaks to peers about making appointments. His 24-year-old friend was recently hospitalized with the virus, and he wants his fellow students to know they’re not invincible.
“Students are seeing this in their friend groups,” he said, after assuming they were “exempt because we’re not 55 and older.”
There are signs that vaccine demand across the state is growing. Last week, 71,000 residents received shots, up from roughly 20,000 five weeks earlier.
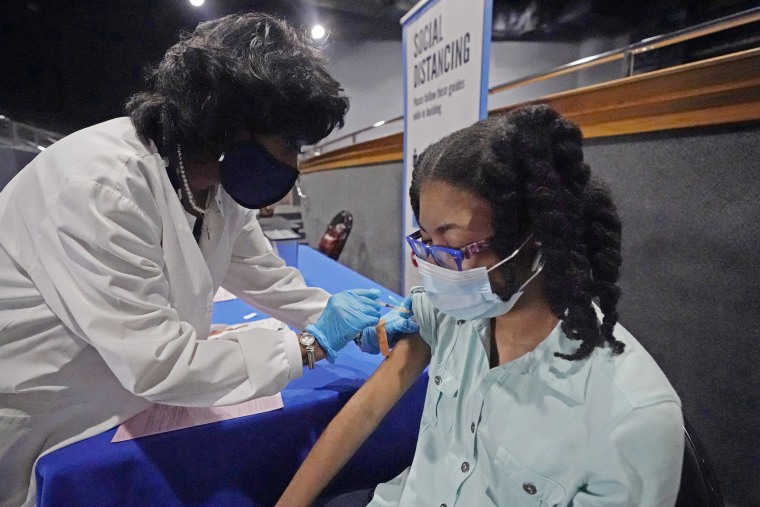
Ian Taylor, 21, was one of the last people in his family to get vaccinated. He received his second dose Tuesday morning at Central Mississippi Health Services, a community health center offering affordable care to underinsured people in Jackson.
Taylor was initially concerned about potential side effects but saw that his loved ones were fine after receiving their shots. The growing presence of unmasked customers at his job at Walmart also gave him a nudge.
“It’s better than me up in a hospital, or possibly being someone who’s not affected by Covid, but putting a loved one in the hospital or on the ventilator because I felt like I was immune,” he said.
That same afternoon, Keiera Dotson, a master’s student at Jackson State University, sat in a folding chair inside a former campus restaurant that was converted to a clinic, waiting to receive her first dose of the Moderna vaccine.
The 23-year-old said she showed up “mainly because I know everybody is coming on campus now — and mainly because my grandparents made me and my mom.”
For weeks, Vanessa Haywood, a nurse practitioner, considered it a decent coronavirus vaccination day if a handful of people showed up for their first shot at one of the small rural clinics she helps oversee for a family practice in the Mississippi Delta.
This spring, the practice cut vaccination days down at one of its clinics from five to one per week as the demand for appointments and walk-in traffic slowed.
Even though Bolivar County has one of the best vaccination rates in Mississippi, with at least half of residents having received their first dose, Haywood questioned if some locals would ever roll up their sleeves.
In mid-July, the need for cajoling began to thin as Covid cases spiked and hospitalizations followed. Some people who were reluctant to receive the vaccine moved from “wait and see” to the front of the line.
“Now, the tables have turned,” Haywood said. “You’re coming and asking us.”
