My life can be divided into distinct halves: the time I am not in pain and the time I am.
It shouldn’t have taken me 13 years to find that support, and it shouldn’t be on the sick to educate themselves.
From the outside, I seem to be always breezy, a glass of wine in hand, celebrating with friends, traveling around the world (in pre-pandemic times), all while executive producing a national news show. And those things do happen. But what most people who see me don't know is that they mostly happen while I am in some level of pain.
My illness, endometriosis, affects 1 in 10 people born with uteruses. And it takes an average of 10 years to be diagnosed. Why? Because there's such minimal knowledge about what the disease actually is. March is Endometriosis Awareness Month, and even though the calendar changes on Thursday, it's vitally important that we continue to keep the focus on this illness the rest of the year — the people who suffer will have no choice but to do so.
The lack of knowledge starts with the definition. Endometriosis is a disease in which tissue similar to what lines the uterus is found outside the uterus. Unfortunately, misinformation saying it's actually the tissue that lines the uterus proliferates. That distinction matters, because the disease needs to be treated as a full-body illness — as the tissue can be found everywhere from the lungs to the brain, causing complications from kidney failure to colon problems — rather than simply as a gynecological condition.
In my case, the pain started when I was 18 and home from freshman year of college for the summer. I remember the pain so vividly. It knocked me off my feet, and I told my parents I couldn't go to a family function. It was the first of so many events I had to miss because of pain, because of what I can only describe as the feeling of barbed wire stabbing me repeatedly inside. Pain is my main symptom, though endometriosis can also cause serious fatigue, food intolerance, infertility, gastrointestinal issues and urinary problems, among a myriad of effects.
When I went to the doctor, she told me that birth control would essentially cure me and suggested a drug called Lupron, which is a commonly prescribed treatment. It made my body mimic menopause, and it was awful. I discontinued the treatment because I decided I'd rather feel the pain than experience hot flashes during class in Arizona. Regardless, hormonal suppression treatments like this one are just Band-Aids that don't address the real problem: the actual disease.
Yet even the governing body of gynecologists recommends birth control and hormonal suppression to begin treating the disease. I've seen even some surgeons get frustrated by this, because it leads so many people to wait years to get formally diagnosed or treated correctly.
For me, it took 13 years. Thirteen years of trips to the emergency room, visits to the doctor, IVs full of pain medication. And every time, the same menu of responses: It's just bad period pain. Or you have a ruptured cyst. And there's nothing to do about it. The clear message was that my disease could be treated through painkillers and other mitigating treatments, while surgery was a radical step.
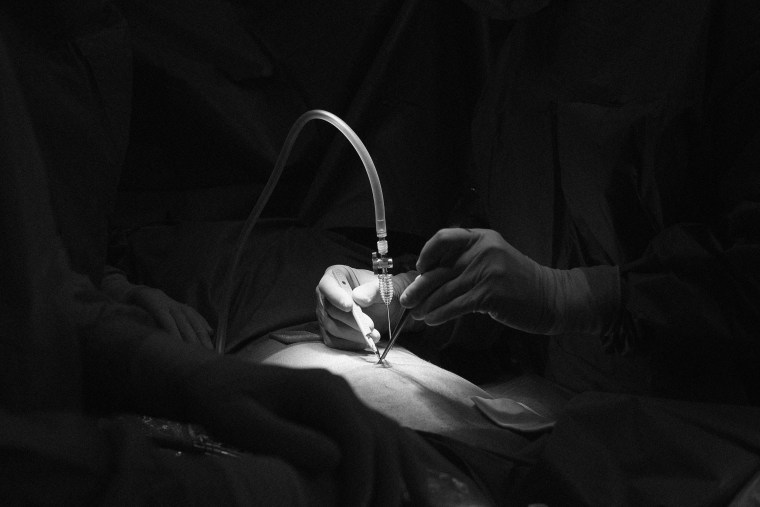
One of the complicating factors is that imaging like MRIs, CT scans and ultrasounds very often don't show the disease, as was true for me. The only way to be formally diagnosed is via laparoscopic surgery, which is expensive and inaccessible to many, since so often insurers see it as a drastic measure they categorize as elective.
Every time I left a hospital or a doctor's office, I felt so frustrated. How was there nothing to be done? How was it OK to just "monitor" it? I felt so invalidated at so many different points in my pain that I resigned myself to having to live with it.
But that changed last fall, when I endured 13 straight days of debilitating pain. I was no longer willing to accept the situation and just power through it. I was going to take control and take my life back. I was on a mission to learn everything I could about treating the illness that afflicted me.
That's when I found out that so many sufferers of this disease did the same: They got their information about their illness on social media and by self-education. That includes Nancy's Nook endometriosis community, which told me about the different surgical techniques and the gold standard of treatment. I learned that a hysterectomy isn't a cure, nor is pregnancy. Both are things I had heard from doctors in the past. Both assume that endometriosis is just a reproductive disease, when, again, it's a full-body disease.
What I needed was excision surgery, a highly skilled technique that cuts the disease out at the root. However, this isn't accessible for many people, because it, too, is usually considered elective. Gynecological surgeons often perform ablation surgery, which burns the endometriosis but doesn't cut it out, meaning symptoms can persist.
On March 1, the first day of Endometriosis Awareness Month, I had my excision surgery. It cost $7,000 (it would've been more than $150,000 without any insurance coverage), and that's on the very low end. This price tag came on top of the thousands of dollars I'd spent on other treatments, specialists, doctors and tests. There simply aren't a lot of surgeons out there who have the expert level of technique needed; my surgeon, who does, removed two dozen disease specimens from multiple organs.
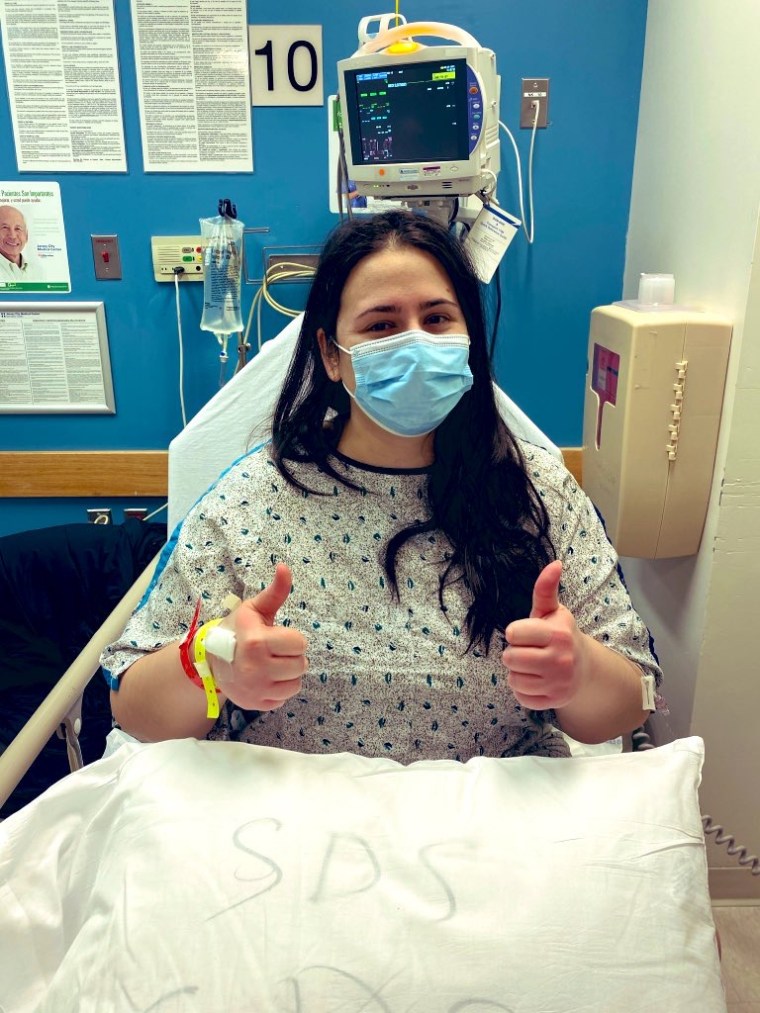
I am so happy to say that I am one month post-surgery, and I feel the best I have in a very long time. I know I will continue to need treatment to support the symptoms I have as a result of this illness, but the debilitating pain has been minimized.
For those suffering and told it's "just a bad period," it's not. Please find a new doctor. Please know you are not alone. Please know it's not in your head. Please know there are compassionate and caring providers who won't question your pain.
It shouldn't have taken me 13 years to find that support, and it shouldn't be on the sick to educate themselves. We need more awareness for a nasty disease that affects an estimated 200 million people worldwide. Even though the calendar is moving past Endometriosis Awareness Month, I won't stop educating others until there's a cure.