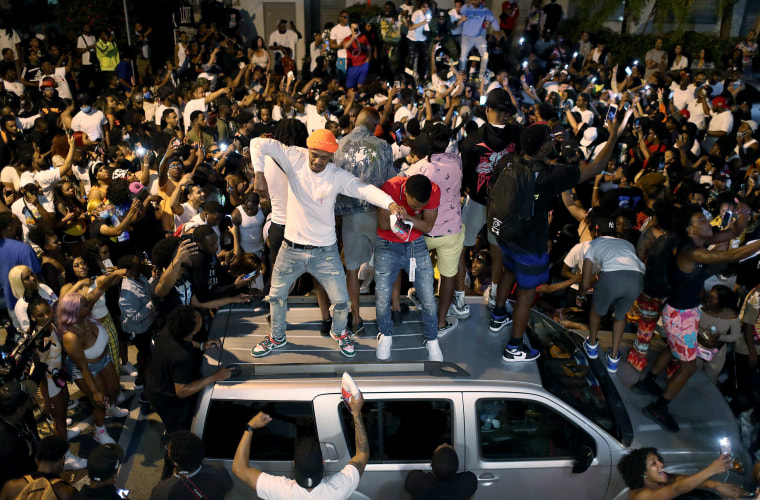The spring break chaos in Miami Beach and the resurgence in Covid-19 cases is leading many to wag their fingers at college students who flooded relatively open Florida and likely brought Covid-19 with them. Instead, we should be wagging our fingers at policymakers.
We have erred by not having placed college students higher on the vaccination distribution list. It is time to rethink that policy, and fast.
First, we should admonish them for not having had the foresight to recognize that young people fed up with social distancing and public health restrictions for more than a year might decide to let loose. Second, they have erred by not having placed college students higher on the vaccination distribution list. It is time to rethink that policy, and fast.
This may seem like an equity problem: Why should state and federal policies privilege the young, healthy and occasionally reckless? Indeed, compared with 18- to 29-year-olds, the rate of hospitalizations for the 40- to 49-year-old population is at least twice as high, and the rate of death is at least eight times higher. Why not give priority to older people who are more likely to get seriously ill?
Such well-meaning equity concerns assume, however, that the young party animals we see in news video from the Sunshine State represent the college-going population. Real college students are much more diverse. For starters, only 56 percent of college students are under age 24. About a third are ages 24 to 39, and 1 in 9 are over age 40.
Moreover, the broader principle in administering vaccine shots equitably is to diminish the risk for those who are most at danger to spread the virus. Vaccinating college students is an effective way to lower that danger, for two major reasons: College students are mobile and spread Covid-19 with them whenever they travel, and they live in congregate living facilities where infection rates are much higher than in other housing setups.
These realities pose a threat to the wider population, with its older and more at-risk groups. The students who went on spring break trips last year often contracted the disease and spread it across the country.
And spring break travel isn't the only type of student movement. Bringing students back to college towns for the reopening of campuses last fall was responsible for thousands of additional Covid-19 cases across the country. In Wisconsin, researchers found that the same strain of Covid-19 that infected college students also infected people in a nursing home. It's estimated that 100 deaths per day in late summer and early fall — nearly all in the 70-plus-age population — were directly related to colleges reopening.
Even when they stay put, college students lead lives that make them risks to one another and the broader community. They often live in congregate facilities like dormitories and fraternity and sorority houses, which are higher-risk environments, just as nursing homes and correctional facilities are. Early work from the University of Colorado shows that roommates from whom students contracted Covid-19 had 6.5 times the viral load of other people.
Colleges can do only so much to reduce transmission. The best tools are to shut down travel, enforce mask-wearing protocols and build out high-quality testing regimes that identify infected students. Around 60 percent of colleges and universities canceled or modified spring break this year to limit student travel, and the University of California, Davis, even paid students $75 to stay on campus, but that did only so much.
Most institutions also have some sort of mask mandate. But very few can afford to test at the needed levels. Given that asymptomatic spread is responsible for at least half of Covid-19 cases, anything less than testing all students all the time is just public health theater.
Yet only 16 percent of four-year colleges and universities have mandatory regular testing of asymptomatic students, according to data from the College Crisis Initiative, which I run at Davidson College in North Carolina. And even some of those institutions use so-called "rapid" tests, in which 1 in 5 cases are likely to be misdiagnosed as false negatives. It costs about $100 per test for higher-quality tests that make fewer mistakes. For a campus of 20,000 students, high-quality testing of every student every week of a normal semester would come to about $30 million.
While campuses don't have the resources they need, states do. They can change the game by moving college students up the priority list. Vaccinations offer a way for students to avoid infecting one another and likely the surrounding communities. Students who receive a vaccine are extremely unlikely to get sick. Early work from Israel, which started vaccinating college- and high-school-age students in January, suggests that vaccination reduces viral load enough to decrease infectiousness and reduce transmission.
If college students are going to take shots in bars during spring break, it's time we make sure they have shots in their arms. Students need to jump to the front of the line for Covid-19 vaccinations even if they don't fall into high-risk groups. Doing so will make them and the communities they visit safer — and allow colleges and universities to reopen for the fall to avoid disrupting more educations and local economies.