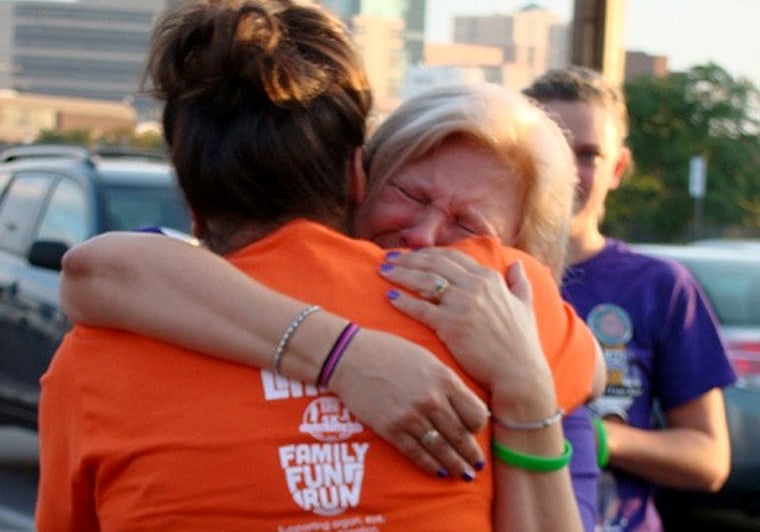
Six months ago, Denise Wagner and Susan Adcock were strangers, two ordinary moms who had no idea that they’d soon be connected by the grief — and hope — of an organ transplant.
On Saturday, the two women and their families will gather for a joint Thanksgiving dinner to mourn the loss of Wagner’s 24-year-old son, Jeremy Baran, who died in June of a drug overdose — and to celebrate the life of Adcock, who received the young man’s heart.
“I prayed that those organs would go to people who were deserving of them,” says Wagner, 50, of Crofton, Md. “She’s such a kind, giving person. We had an instant bond.”
“God gave me Jeremy’s heart because he knew that I would help in her grieving,” says Adcock, 55, of York, Pa. “I have a piece of her love.”
Wagner and Adcock are an example of what organ transplant experts say is a small but growing phenomenon: Families of donors who form close ties with the recipients of their loved ones' organs.
“These are incredibly powerful meetings,” says Sharon Ross, director of community outreach for Lifesharing, a non-profit Organ Procurement Organization, or OPO, in San Diego, Calif. “We find it very cathartic for the families that do it.”
More than 14,000 people donate organs in the U.S. each year, either after death or while they’re still living, according to data from the Organ Procurement and Transplantation Network. Each donor can help up to eight people with organs such as the heart, lungs, pancreas and kidneys and a dozen or more through tissue donation.
That may create the opportunity in theory for tens of thousands of donor families and recipients to connect, but in practice, it’s very rare, says Ross.
“Nationally, it happens in only 5 percent of cases. Both sides have to agree to meet. It’s kind of a courting,” she says.
Part of that is because of the strict anonymity rules that govern donation. Direct communication is not allowed; organ donor families and organ recipients who want to reach out have to send letters of introduction through the OPOs or transplant centers, which forward them along and monitor the communication.
That’s because of longstanding worries about the emotional impact of such meetings and the possibility of potential coercion, said David Lewino, a pre-transplant nurse at the University of California San Diego Health System who has studied interactions between donor families and recipients.
“When I started, it was taboo,” said Lewino, who has been working in the transplant field for 30 years. “There was this feeling that you can’t have recipients and donors meet, you just can’t. There was a general concern that there was going to be some type of quid-pro-quo from the donor to the recipients.”
Even today, many OPOs are reluctant to encourage donor families and recipients to meet, Ross and others say. And, truth to tell, most donor families and recipients don’t want any contact after the transplant takes place.
“Some people choose never to respond. It’s too hard,” she says.
For donor families, the transplant recipient may be a painful reminder of what they’ve lost. For recipients, there’s often a feeling of guilt at benefiting from someone else’s death.
“How do you say thank you to the person who has lost everything and saved your life in the midst of their hell?” Ross says.
But those who’ve chosen to meet, despite the potential for more pain and heartache, say it’s worth it.
“It’s been really healing for me,” says Wagner, who was bereft after Jeremy overdosed on heroin during a relapse from rehab treatment. Her son, whom she describes as a lively daredevil and "cute as a button," was designated as an organ donor on his driver’s license, something Wagner didn’t know.
“To know that he was able to save not just one life, but five lives, helps,” she says.
Wagner agreed to meet Adcock — a caterer and chef with five children and six grandchildren — after Adcock sent a seven-page letter. The pair, who met at an October charity fun run to benefit organ donation, say they were both nervous.
“When I hugged her, I could feel his heart,” Wagner recalls. “I could feel it pounding. It was hard to let go.”
For her part, Adcock says she felt compelled to reach out to Wagner because they were both mothers with children close in age. "I was relating to that, from a mother's aspect: If this was my child, if I lost my son, I would want to know."
She says she “talks” to Jeremy daily and thanks him for the sacrifice that saved her life. And she communicates with Wagner by phone or text at least a few times a week.
“My main reason for doing it was to let them know I was doing well, and I was taking the best, best care of his heart,” Adcock says.

Knowing what happened to the recipients — and that they’re doing well, is crucial for parents like Teena Webster, 52, who has contacted six of the seven people who received organs from her 20-year-old son, Aaron, who died in a September 2009 car crash in Arkansas. In addition, he donated his corneas and grafts of skin that have been used for 200 children who suffered severe burns or accidents.
“It’s his one life traded for many others,” Webster says. “It doesn’t take away my missing him, but I can rationalize it.”
The same goes for Alicia Stillman, 50, of West Bloomfield, Mich., whose 19-year-old daughter, Emily, died in January after a sudden meningitis infection. Stillman has met the men who received Emily’s kidney and lung — and the 34-year-old doctor, Guy Mulligan, who received her heart.
“He sat down on the couch that Emily would lay on when she would watch TV,” Stillman says. “He let me lay my head on his chest. I felt her heart beating against my ear. I heard her heart beating strong.”
Mulligan, who lives in Aurora, Ohio, is the father of two young children ages 6 and 4 and is expecting a baby — conceived after his heart transplant — in January.
“These people are meant to do something good,” Stillman says. “We joked around with him: We think you got the heart because you’re going to find the cure for diabetes.”

Mulligan, for his part, says that agreeing to meet his donor’s family was the least he could do. “It’s difficult. It’s like simultaneous joy and guilt at the same time,” he says, adding. “It would be a little bit selfish for me not to acknowledge that I’m able to go on because there was a sacrifice.”
Still, such successful cases are not necessarily the norm, says Art Caplan, head of the division of medical ethics at New York University Langone Medical Center. Organ transplant is an intensely emotional endeavor for all parties. There’s a reason relations between donor families and recipients are — and should be — carefully monitored.
“I wouldn’t say it’s right for everyone,” he says. “Even though the donor might want to meet the recipient. There’s a chance that the donor families will want to work themselves into their lives. You get unwanted emotional overtures. Even a tinier percentage of people start to think, ‘You owe me something.’ Those are all reasons why anonymity is the default, is presumed.”
Adcock says she knows all about such concerns. But she says she also knows that Wagner will bring a stethoscope when she comes to dinner on Saturday and that it will comfort the grieving mother to listen to her son’s heart.
“Some people are afraid to reach out,” says Adcock. “If I didn’t reach out, I’d never know. I just wish more people would be aware of what can come out of this.”
JoNel Aleccia is a senior health reporter with NBC News. Reach her on Twitter at @JoNel_Aleccia or send her an email.