As the huge baby boomer generation surges toward retirement age, an unsettling issue grows ever more pressing: finding the work force to tend to the millions of boomers who will someday need ongoing care because of physical and mental frailties.
Alarm is spreading across the health care sector in the face of stark demographics.
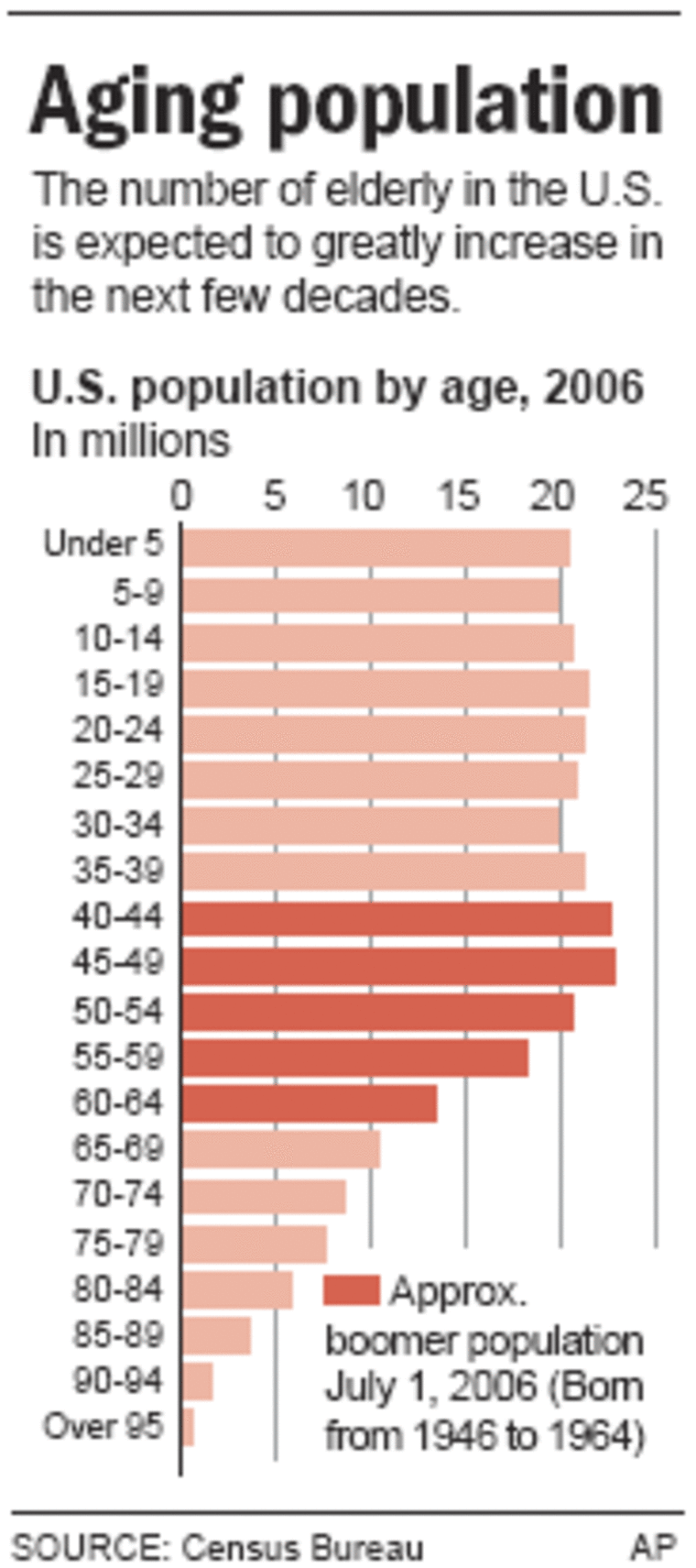
There will be an enormous increase in America’s elderly population in the next few decades, while the traditional labor pool for caregivers — women from their mid-20s to mid-50s — will scarcely grow at all, compounding problems for a work force already beset by low wages and high turnover.
Federal statistics suggest that roughly 3 million people work in direct-care jobs, mainly with the elderly, as nursing assistants, home health aides and personal care aides. Experts project there will be demand for nearly 1 million more of these workers in the next decade, and perhaps a total of 3 million more by 2030 — when all surviving members of the 78-million-strong boomer generation are older than 65.
Direct-care workers “are the hands, voice and face of long-term care for millions of elders,” said Steven Dawson, president of the New York-based Paraprofessional Healthcare Institute.
“And yet, the long-term care system has simply presumed that an endless supply of workers ... will always be available to transfer our mothers from bed to wheelchair, or to feed our fathers, no matter how little we pay these workers, or how poorly we supervise them, or whether we even have the decency to offer them health insurance.”
Wages for these jobs, as of 2005, averaged less than $10 per hour, and a quarter of the work force had no health insurance. Groups advocating for better compensation were stunned this week when the Supreme Court ruled unanimously that the nation’s 1 million home-care workers are not entitled to overtime pay under federal law.
The ruling “underscores how unprepared we are to care for the millions of seniors who will want to live at home instead of institutions,” said Gerry Hudson, a vice president of the Service Employees International Union. “If we are to avert a home-care crisis, we must invest in living wages and health care coverage.”
SEIU already represents about 400,000 caregivers; it hopes to expand those ranks by touting its success in states such as California, where extensive unionization has been followed by higher pay and lower turnover.
But Hudson acknowledges that caregiving differs from most industries — strikes would be a desperate last resort because of the potential harm to elderly clients, and there is some common cause with employers on the need for broad changes in how America finances long-term care.
That kind of overhaul may be far away; in the meantime, many proposals and projects have emerged.
Some states are providing health coverage for uninsured caregivers. Community colleges, with funds from state agencies and the Labor Department, are beefing up training programs for home-care workers. Vermont is experimenting with a Choices for Care program in which it pays any caregiver — including a friend or relative — $10 an hour to tend to an elderly person who might otherwise be forced to a nursing home.
The nursing home industry has distinct labor problems of its own, with close to 100,000 vacancies for nurses and nursing aides, and an annual turnover rate of 70 percent as some nurses quit the profession and others take higher-paying jobs at hospitals.
The American Health Care Association, which represents thousands of nursing homes, says the cost of high turnover — notably recruiting, training and using temporary contract workers — exceeds $4 billion a year.
Ken Preede, the association’s director of government relations, hopes the current debate over immigration leads to changes that could ease the nursing shortage.
Already, thousands of nurses from India, the Philippines and elsewhere work at U.S. nursing homes despite sometimes cumbersome visa procedures. Preede would like to see immigration changes that would make it easier to fill such specialized, high-need positions and also to recruit guest workers for less-skilled nursing home jobs.
Pamela Doty, a policy analyst with the Department of Health and Human Services, said the caregiver gap often is most acute in rural areas with few immigrants. She cited Kentucky and Arkansas as states with notable challenges.
In areas short of caregivers, the consequences can be painful. Some elderly people must make do with ill-trained and overburdened helpers; others who would prefer to live on their own are forced into the more costly option of nursing homes. Even when family members step in, as millions do, there is a price emotionally, physically and often financially if career duties are disrupted.
“Many families are committed to keeping their relatives in the community, so they’ll do their utmost — but it takes a toll on them,” Doty said.
There are some optimists.
Patricia Kappas-Larson, a nursing expert with the Evercare health plan, believes caregivers can be trained to be more skilled, more motivated and more flexible in finding ways to serve the elderly outside of hospitals and nursing homes. Emily DeRocco, the Labor Department’s assistant secretary for employment and training, predicts the baby boomers — many of them now caring for aging parents — will ensure that the market economy produces enough qualified caregivers for their own retirement era.
But Dr. Richard Butler, president of the International Longevity Center-USA, is less confident — fearing that severe problems will persist until America figures out a way to include long-term care as part of basic, affordable health care coverage.
“My impression is that baby boomers haven’t really addressed the issues of aging yet — they’re more absorbed with how to avoid aging,” he said. “We’re facing a historic demographic change, and we do not have an adequate, well-trained work force — from doctors down to basic in-home caregivers — who know the details of aging.”
