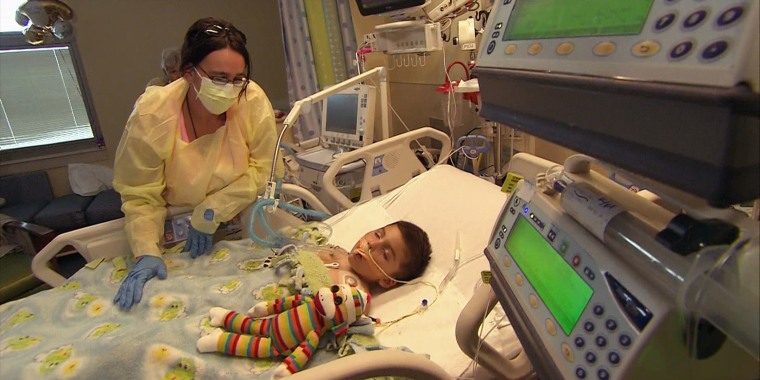
Dr. Riley Bove knows about nerve damage. She’s a neurologist, specializing in multiple sclerosis and trained at top medical schools.
Yet Bove had to fight to get help for her son Luca in 2014 when he developed what’s now known as acute flaccid myelitis — the polio-like syndrome that paralyzes or weakens muscles, sometimes permanently.
Bove and two other parents described their ongoing struggles with AFM, from getting doctors to take their children’s symptoms seriously to the day-in and day-out slog of treating children with crippling and irreversible nerve damage. They decry delays in research that could lead to better treatments and the continued lack of education about the problem across the medical profession.
Four years after it was first widely identified, acute flaccid myelitis remains a challenge to doctors and public health officials. The Centers for Disease Control and Prevention said it looks very much like a virus — probably more than one — that is either attacking the nerves or setting off an autoimmune reaction that damages nerves. But the CDC says there is still not a single clear cause for the condition, which has been conclusively diagnosed in 116 patients so far this year.
“We demand more from the CDC with respect to rapid case ascertainment (including cases before 2014) and movement toward a vaccine,” Bove and her fellow parents write in a letter to the journal JAMA Pediatrics.
“Second, when we brought our children with new weakness for evaluation by their pediatrician, or an acute care clinician, most of our children never underwent a neurological evaluation,” they added. “Acute limb flaccidity is typically obvious, yet many of us were told, ‘He is weak from his fever,’ or even, ‘It’s in her head.’ This led to delays in evaluation, neuroimaging, and swabbing for possible infectious pathogens.”
Bove, who has been in touch with hundreds of other parents, says her experience is typical.
“We all got sick — the whole family, the preschool, everybody got sick with fevers and coughs and colds,” Bove, now a neurologist at the University of California San Francisco, told NBC News.
“We all got over it.” But Luca’s fever came back. “He woke up with a very weak neck and right arm,” Bove said. Bove was finishing her qualifications at Harvard Medical School and knew these signs meant Luca needed immediate medical attention. But she was also cautious about second-guessing her child’s physician, and did not push back when Luca’s regular pediatrician seemed unconcerned.
“He was dizzy and weak. He couldn’t climb onto the examination table in the doctor’s office,” Bove said. “They still didn’t do a neurological exam.”
When Luca’s symptoms failed to resolve as the day went on, Bove sent him back for a second check. Again, he was sent home. By that evening, she was worried enough to send a video to a friend at Boston Children’s Hospital. Acute flaccid myelitis had been making headlines for several weeks, and the friend immediately suspected it might be affecting Luca. That’s when all the stops were pulled out.
“We got him in to Boston Children’s,” Bove said. “We got everything expedited, the diagnosis within 24 hours and started aggressive treatment. Despite that he started to get worse and worse. By the eighth day, he was paralyzed from head to toe.”
None of the treatments worked. Doctors tried steroids, infusions of antibodies and a blood treatment called plasmapheresis, as well as an antiviral drug. It was months before Luca could walk again and now he has permanent nerve damage that has stopped the growth of his right arm and shoulder. He looks, Bove said, like a polio survivor, although the CDC and other experts are confident polio is not causing the syndrome in these kids.
Now Luca wears a neck brace and attends some sort of therapy three to four days a week. “Physically, he can’t keep up with his friends,” Bove said.
Bove wants parents to know to be on the lookout for what is still an extremely rare condition. Only 440 cases have been verified since 2014, according to the CDC.
“We grieve those final days when our still-normal children climbed their last playground structures or took their last runs down the block or their last independent breaths,” Bove wrote along with Erin Olivera, a Los Angeles registered nurse whose son developed the syndrome in 2012 and Heather Werdal of Bremerton, Washington, whose son Hayden was affected in 2014.
If such well-informed professionals are struggling, Bove said, parents with little or no medical knowledge and fewer resources are at even more of a disadvantage.
“I am a Harvard-trained neurologist with all this access,” Bove said. “My kid is vaccinated. We are insured. I trained with the people who are in the know about AFM.”
Most patients with AFM have suffered from what appears to be a viral infection, the CDC said. “Yet, as connected as we are, we can’t find the bug,” Bove said. “We don’t know long-term outcomes. We don’t know how to promote bone growth,” she added. “We know so little and everyone’s a little bit in the dark.”
Researchers such as Dr. Kevin Messacar of Children’s Hospital Colorado say they’ve identified at least two viruses that can cause the condition: EV-D68, which normally causes symptoms resembling the common cold, and EV-A71, which can cause hand, foot and mouth disease. Polio virus is the most notorious cause of AFM-like conditions, but polio no longer circulates in most of the world, especially not in the U.S., and none of the AFM patients has had polio.
Separately in the same journal, Messacar and fellow researchers who have built their own network to study AFM and share information about it point out that sometimes the symptoms of the syndrome are easy to miss. “When AFM is suspected, hospital admission is recommended because patients may experience rapid deterioration of weakness to respiratory compromise,” they wrote. Some children may need to go straight to intensive care because of the risk that they may quickly develop trouble breathing.
It’s also important to know what is and what isn’t AFM, because conditions that resemble AFM can sometimes be treated.
Three of the experts analyzed the records of 45 patients suspected to have AFM and found many instead had transverse myelitis, which can be treated with immune suppressants, or spinal cord stroke. A few had Guillain-Barre syndrome, a condition called Chiari I myelopathy or meningitis.
“Those patients with definitive AFM had a fever or viral infection before the onset of weakness in the arms or legs,” they wrote. “They also lost function of their limbs on one side of the body first with the majority of children losing function of a single limb or all four eventually.” Doctors need to be on the lookout for these symptoms, they advised.
There may be a treatment that could help, they said. “Children with AFM respond better with infusions of immunoglobins — a collect of antibodies that can help tag pathogens as invaders so the immune system can eliminate them,” they wrote. “This is an area in urgent need of further research.”
Sen. Kirsten Gillibrand, D-N.Y., has asked her colleagues to appropriate $1 billion by the end of the year to the CDC for its new task force aimed at addressing AFM.