Researchers in Boston are on the verge of what they say is a major advancement in lung cancer screening: Artificial intelligence that can detect early signs of the disease years before doctors would find it on a CT scan.
The new AI tool, called Sybil, was developed by scientists at the Mass General Cancer Center and the Massachusetts Institute of Technology in Cambridge. In one study, it was shown to accurately predict whether a person will develop lung cancer in the next year 86% to 94% of the time.
The Centers for Disease Control and Prevention currently recommends that adults at risk for lung cancer get a low-dose CT scan to screen for the disease annually.
But even with regular screening, the most skilled radiologist’s eye can’t spot everything — and that’s where Sybil comes in.
“The naked eye cannot see everything,” said Dr. Lecia Sequist, an oncologist and the program director of the Cancer Early Detection and Diagnostics Clinic at Massachusetts General Hospital. “The AI that we developed is looking at the scan in a completely different way than a human radiologist looks at it.”
The tool, experts say, could be a leap forward in the early detection of lung cancer, the third most common cancer in the United States, according to the CDC. The disease is the leading cause of cancer death, according to the American Cancer Society, which estimates that this year there will be more than 238,000 new cases of lung cancer and more than 127,000 deaths.
Sybil is not yet approved by the Food and Drug Administration for use outside clinical trials, but if approved, it could play a unique role.
There are more than 300 AI tools approved by the FDA for use in radiology, according to Anant Madabhushi, a professor in the department of biomedical engineering at the Emory University School of Medicine in Atlanta. Most are used to assist doctors in the diagnosis and treatment of cancer, he said, but not for predicting someone’s future cancer risk, like Sybil does.
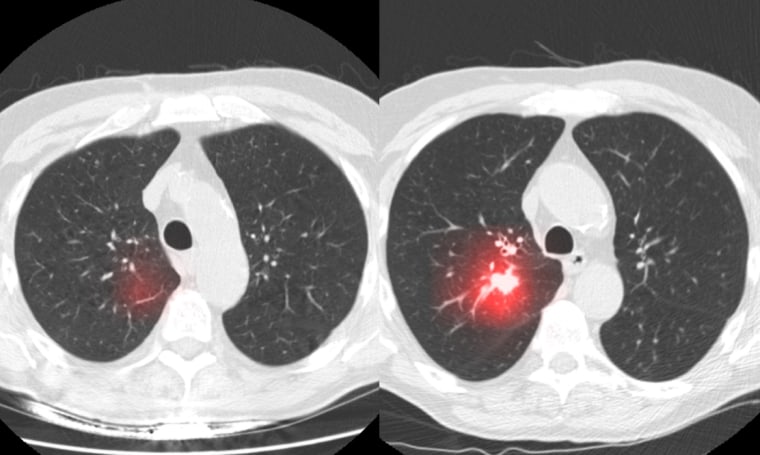
Sybil looks for signs of where cancer is likely to turn up, so doctors know where to look and can then spot it as early as possible.
Lung cancer is most treatable when detected early, said Dr. Kim Sandler, an associate professor of radiology at Vanderbilt University Medical Center in Nashville, Tennessee.
But early detection is difficult, she said. Since the lungs can’t be seen or felt, the only way to spot it early is with a CT scan. By the time symptoms appear, including persistent coughing or trouble breathing, the cancer is usually advanced and the most difficult to treat.
Past research has shown that screening with low-dose CT scans can reduce the risk of death from lung cancer by 24%, because they can help detect cancer sooner, when it’s more treatable.
But an AI tool could potentially increase the rates of early detection of lung cancer — and potentially increase survival rates as well, Sandler said.
“This is great for radiologists, but more importantly, it’s really great for our patients to be able to give them that tool to tell them whether or not we think something is lung cancer,” she said.
How does Sybil work?
To predict cancer risk, Sybil relies on a single CT scan. It analyzes the three-dimensional image, looking for not only signs of abnormal growth in the lungs, but also other patterns or nuisances that scientists don’t fully understand yet, said Dr. Florian Fintelmann, a radiologist at Mass General Cancer Center and one of the researchers working on Sybil.
Based on what it sees, Sybil provides predictions for whether a person will develop lung cancer in the next one to six years, he said.
There have been cases, Fintelmann added, where Sybil has detected signs of cancers that radiologists did not detect until nodules were visible on a CT scan years later.
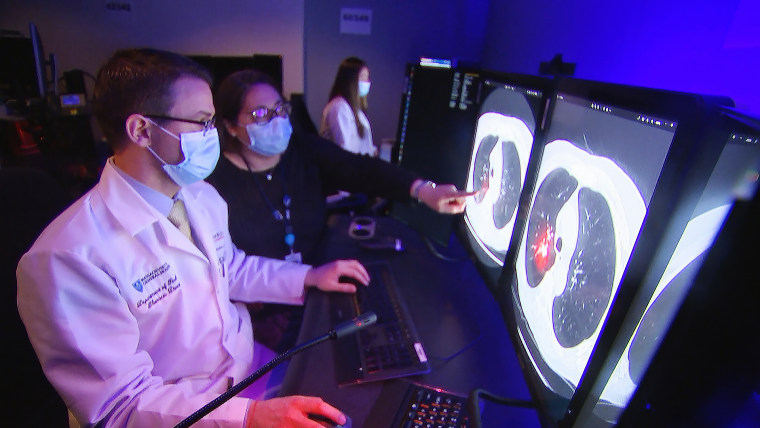
Fintelmann said he sees a future in which the AI tool is helping radiologists make important treatment decisions — not replacing radiologists altogether.
“The future of radiology is going to be AI-assisted,” he said. “You will still need a radiologist to identify where the cancer is, identify the best possible treatment and actually do the treatment.”
AI, however, is still far from perfect.
One issue that Madabhushi, of Emory University, said he worries about is the type of data being used to train AI.
“A lot of data that comes from medical institutions or clinical trials do not represent the diversity of our country,” he said, adding that he believes the AI tools are not being developed in a way that is tailored to help Black and brown people.
The scientists who developed Sybil have acknowledged that the data used to create the AI tool does not include “sufficient Black or Hispanic patients to have confidence in broad applicability yet.”
The FDA has already taken a step to address this issue, announcing last year that it would soon require researchers and companies seeking approval for medical products to submit a plan that ensures diversity in clinical trials.
“We have to make sure that AI does not reflect or capture our biases,” Madabhushi said.
There are also concerns about overdiagnosis, Sandler said. Doctors may put patients through a potentially unnecessary biopsy for a nodule that may end up being benign.
“Are we finding cancer that maybe we don’t need to find?” she said.
Follow NBC HEALTH on Twitter & Facebook.



