When Surgeon General Jerome Adams issued an advisory calling for more people to carry naloxone — not just people at overdose risk, but also friends and family — experts and advocates were almost giddy.
This is an “unequivocally positive” step forward, said Leo Beletsky, an associate professor of law and health sciences at Northeastern University.

And not necessarily a surprise. Adams, who previously was Indiana’s health commissioner, was recruited to be the nation’s top doctor in part because of his work with then-Gov. Mike Pence, now the vice president. In Indiana, Adams pushed for harm-reduction approaches, which included expanded access to naloxone and the implementation of a needle exchange to combat the state’s much-publicized HIV outbreak, which began in 2015 and was linked to injection drug use.
Others cautioned, though, that his have-naloxone-will-carry recommendation is at best limited in what it can achieve, in part because the drug is relatively expensive.
Kaiser Health News breaks down what the advisory means, experts’ concerns and what policy approaches may be in the pipeline.
Many public health advocates applaud the surgeon general’s position.
Naloxone, which is a drug that can keep drug users alive by reversing opioid overdoses, is viewed by many as the cornerstone of the harm-reduction approach to the epidemic. Experts say people with addiction problems should carry it, and so should their family, friends and acquaintances.
“We want to put it more in reach,” said Traci Green, an associate professor of emergency medicine and community health sciences at Boston University, who has extensively researched the opioid abuse crisis. “It could not have been a better endorsement.”
Others, including Diane Goodman, who penned a recent Medscape commentary reflecting on the advisory, wonder whether this is a “rational” response to the scourge, since opioid addiction is one of many health problems people might encounter in everyday life and for which treatment options are still limited.
“I'm not sure it makes much more sense than any of us carrying a bottle of nitroglycerin to treat patients with end-stage angina,” wrote Goodman, an acute-care nurse practitioner, referring to chest pain.
“What, exactly, are we offering to addicts once their condition has been reversed?” she asked, noting that without treatment and therapy programs that help wean people from addiction “the odds of survival for any length of time remain low, no matter how much reversal medication is kept nearby.”
Results would likely be limited by naloxone’s price tag.
Take Baltimore, which has been hit particularly hard by the opioid epidemic. Its health department already has pushed for more people to carry naloxone.
But the drug’s price is an issue, said Dr. Leana Wen, the city’s health commissioner, and an emergency physician. She suggested that the federal government negotiate directly for a lower price, or give more money to organizations and agencies like hers so they can afford to maintain an adequate supply.
“Every day, people are calling us at the Baltimore City Health Department and requesting naloxone, and I have to tell them I can’t afford for them to have it,” Wen said.
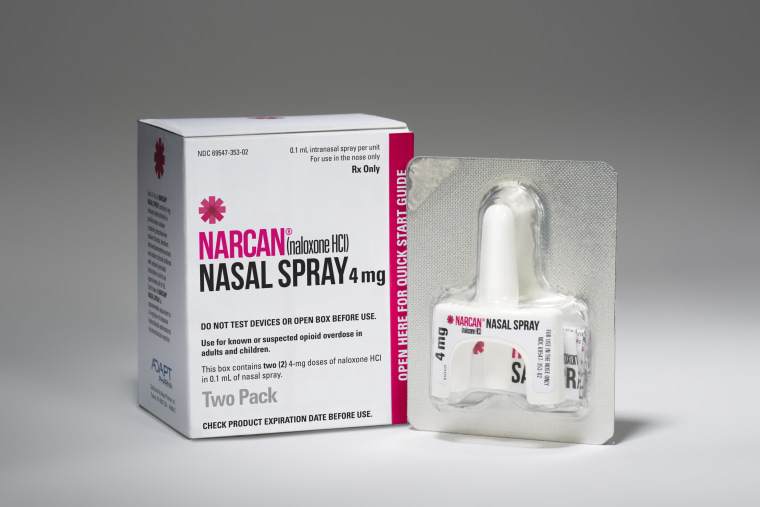
The drug is available in generic form, which can be stored in a vial and injected via a needle, as well as in patented products, such as the nasal spray Narcan, sold by ADAPT Pharmaceuticals, and Kaleo’s Evzio, a talking auto-injector.
Generic naloxone costs $20 to $40 per dose. Narcan, the nasal spray, costs $125 for a two-dose carton, according to ADAPT’s website. A two-pack of Evzio costs close to $4,000, according to GoodRx.
Health departments and first responders qualify for a discounted rate of $75 per carton of Narcan. Kaleo has made Evzio coupons available to consumers, so that some will not have a copay, and it advertises a discount for federal and state agencies.
Skeptics point out that similar methods have been used to build brand loyalty and potentially make a particular product a household name. That’s how Epi-Pen became synonymous with epinephrine for the treatment of anaphylactic shock.
“There’s clearly some overlap” here between the pricing strategies used by naloxone manufacturers and Epi-Pen distributor Mylan, said Richard Evans, co-founder of SSR Health, which tracks the pharmaceutical industry.
But it’s not a perfect comparison. The presence of low-cost generics changes the calculus, he said, as does the different level of demand.
Nonprofit organizations and health care providers keenly feel the pressures of increasing demand and cost.
Experts say price breaks on naloxone are not sufficient to cover the costs on the ground.
“Sixty-four thousand people lost their lives [nationally in 2016] — that’s someone every 12 minutes,” said Justin Phillips, executive director of Overdose Lifeline, an Indianapolis-based nonprofit. “Ten free kits is not going to be enough.”
Phillips said her organization relies on generic naloxone, which is the least expensive formulation. It’s the only feasible option, using dedicated grant money the group received from the state attorney general’s office as part of a program funded by a settlement with pharmaceutical companies.
But that money is almost dried up. “We need to be able to access naloxone — which I’m told is pennies to make — for the pennies it cost to make it,” Phillips said.
Phillips, who worked with Adams when he ran Indiana’s health department, said she has discussed the need for naloxone funding with the surgeon general, but never its price.
Pharmacies assess the hurdles of distribution.
Local pharmacies are key in this chain, but the overdose antidote is new territory for many pharmacists, said Randy Hitchens, the executive vice president of the Indiana Pharmacists Alliance. He said in 2015, when Adams began his push to get naloxone into the hands of drug users and their families, only one or two retail pharmacies carried it.
“This has always been an emergency room drug. Retail pharmacists typically were not used to dealing with [it],” Hitchens said. “A lot were probably saying, ‘What in the devil is naloxone?’”
“Sixty-four thousand people lost their lives [nationally in 2016] — that’s someone every 12 minutes.”
Today, he estimates 60 to 70 percent of Indiana’s more than 1,100 retail pharmacies carry the drug. Walgreens, the pharmacy chain, has committed to stocking Narcan.
Access, though, is always subject to retail pressures.
“If pharmacies are not seeing a steady stream coming in asking for it, they won’t be incentivized to carry it on their shelves,” said Daniel Raymond, the deputy director of policy and planning for the Harm Reduction Coalition.
A patchwork of other decentralized sources for naloxone exist: syringe-exchange vans, county and state health departments, churches and community centers, all trying to find ways to get overdose medication into the hands of people who need it.
That supply stream “meets people where they are,” Raymond said, but those little programs don’t have the muscle to negotiate discounted prices.
“Individual health programs are trying to navigate the crisis on their own, but when you see … growing demand and limited supply, it’s a role for federal intervention,” Raymond said.
He’d like to see the federal government step in to negotiate prices where smaller programs can’t.
The surgeon general’s message is one part of Washington’s broader response to the epidemic. But even as Congress crafts an opioid epidemic response package, it’s not clear it will tackle these concerns.
In the House of Representatives’ Energy and Commerce Committee, one bill being discussed would require all state Medicaid programs to cover at least one form of naloxone. Currently, not all state Medicaid programs do so.
A Senate bill would authorize $300 million annually to equip first responders with naloxone.
But critics say those approaches still don’t address the underlying problems: cost and funding.
“You can either make naloxone available, at a much discounted price, or we need to have a lot more resources in order to purchase it,” Wen said. “I don’t care which one. My only concern is the health and well-being of our residents.”
This story was written by Shefali Luthra and Rachel Bluth and contributed by Kaiser Health News, a national health policy news service that is an editorially independent part of the Henry J. Kaiser Family Foundation, a nonprofit, nonpartisan health policy research and communication organization not affiliated with Kaiser Permanente.