Most women are aware that a family history of breast cancer increases their risk of the disease, but far fewer understand that extremely dense breasts can pose a greater risk.
A survey published Monday in the journal JAMA Network Open found that of nearly 1,900 women who participated, the majority saw breast density as a less consequential risk factor than family history.
But women with extremely dense breasts, which are characterized by minimal fatty tissue, face a risk of breast cancer four times higher than women with the lowest breast densities, according to the study. About 10% of women who get mammograms have this level of breast density. By comparison, having a mother, sister or daughter who's had breast cancer is associated with double the risk of the disease.
Women who have a substantial amount of dense breast tissue but not to an extreme degree — about 40% of those who get mammograms — have a 20% higher risk of breast cancer relative to those with average breast density, according to the study.
That’s slightly lower than the risk associated with having a glass of wine each night, according to Dr. Phoebe Freer, chief of breast imaging at the University of Utah's Huntsman Cancer Institute, who wasn't involved in the survey.
"Everybody has a different amount of fibroglandular tissue and a different pattern," Freer said, referring to dense breast tissue. "It’s almost like a patient’s fingerprint."
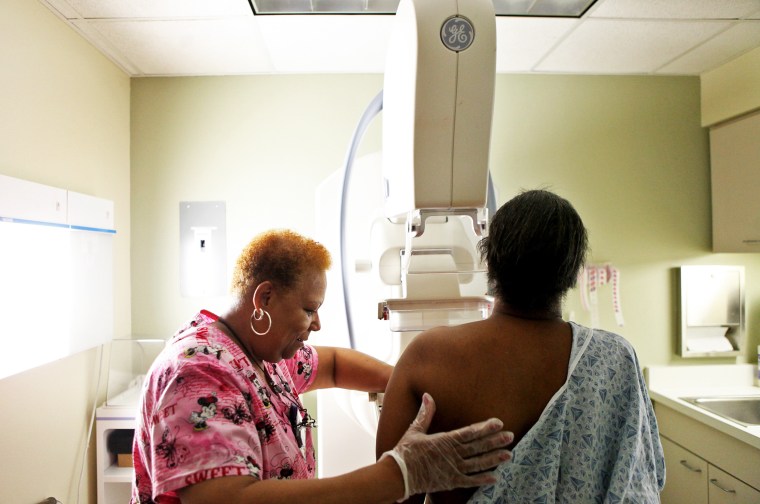
The only way to tell if you have dense breasts is via a mammogram, which doctors generally recommend every one or two years for women starting in their 40s or 50s.
The Food and Drug Administration proposed a rule in 2019 that would require mammography facilities to inform patients about their breast density and its significance. In October, the FDA said it was optimistic that the final rule would be published by early 2023.
Thirty-eight states already require providers to give women information about breast density after a mammogram, but not all of them require providers to notify a woman if she herself has dense breasts.

Since dense breasts are common, doctors may inadvertently downplay the risks, said Christine Gunn, a researcher at the Dartmouth Institute for Health Policy and Clinical Practice, who conducted the JAMA research.
"There are a lot of conversations with primary care doctors where they say, 'This is normal.' For some women, it translates to, 'Oh, I don’t have to worry about that,'" Gunn said.
In individual interviews as part of Gunn's survey, six out of 61 women said dense breasts contributed to breast cancer risk.
There are two reasons dense breasts are linked to a higher risk of breast cancer.
First, the composition of the breast might predispose people to cancer. The reasons for that aren’t clear, but scientists suspect that cancer is more likely to develop in fibroglandular tissue, which is unique to the breast, as opposed to fatty tissue, which is found throughout the body.
Second, because women with extremely dense breasts have almost all fibroglandular tissue, it's harder to detect cancerous masses or calcium deposits on a mammogram. That makes it easier for cancer to grow or spread undetected rather than being spotted and treated early.
Checking for cancer in a patient with dense breasts is like searching for a white spot on a white wall, according to Dr. Melissa Durand, an associate professor at the Yale School of Medicine Department of Radiology and Biomedical Imaging.
Durand explained that both fibroglandular tissue and cancer show up white on a mammogram, whereas fatty tissue shows up black.
"In a completely fatty breast — so lots and lots of black on the mammogram — we can be as accurate as 98%," she said. "But our sensitivity can drop really low — in some studies, even as low as 30% — if you have an extremely, extremely dense breast."
Radiologists said the ideal type of mammogram, especially for women with dense breasts, is a digital breast tomosynthesis, which is often better at detecting cancer than standard mammograms.
From there, doctors might recommend an ultrasound or MRI. Women with dense breasts should probably get supplemental screenings each year, radiologists said.
Ultrasounds are safe and relatively inexpensive, but Freer said they can miss cancer or show false positives, which can be confusing for patients. MRIs are the most sensitive option, but to get insurance companies to cover the cost, patients usually need to show additional risk factors, such as a genetic mutation or family history of breast cancer.
"The more often you get screened, the more likely you are to be called back for additional imaging," Freer said. "It does create some anxiety and it definitely takes time. Most patients are willing to undergo that risk in order to get the life-saving benefit."
Women can't change their breast density, but it can shift with age.
"Typically, younger women will have denser breasts," Durand said. "As we age, just like other parts of our bodies, we acquire more fat, so your breast tissue can get more fatty tissue in it."
To lower one's risk of breast cancer overall, doctors recommend limiting alcohol intake, exercising regularly and maintaining a healthy diet. The Breast Cancer Surveillance Consortium offers an online tool to help people gauge their breast cancer risk based on multiple factors, including breast density.