The biggest study ever of calcium and vitamin D supplements for older women showed they offered only limited protection against broken bones, raising questions over what has been an article of faith among doctors and nutritionists.
The supplements seemed to reduce the risk of broken hips in women over 60 and also helped those who took the supplements most regularly. But as to preventing bone fractures overall, vitamin D and calcium flunked in these healthy women.
One of the researchers, Dr. Norman Lasser at New Jersey Medical School, said the study is "not as ringing an endorsement of calcium as one might like."
Even so, many experts said they would stand behind federal guidelines recommending the supplements, if needed, to meet standard intake of calcium and vitamin D.
"There's probably a small benefit," said Dr. Joel Finkelstein, of Massachusetts General Hospital, who wrote an editorial in the New England Journal of Medicine where the study appeared Thursday. "It's a good start, but women at higher risk need to know it's not enough."
The findings were an offshoot of the big national study of diet and hormone therapy known as the Women's Health Initiative.
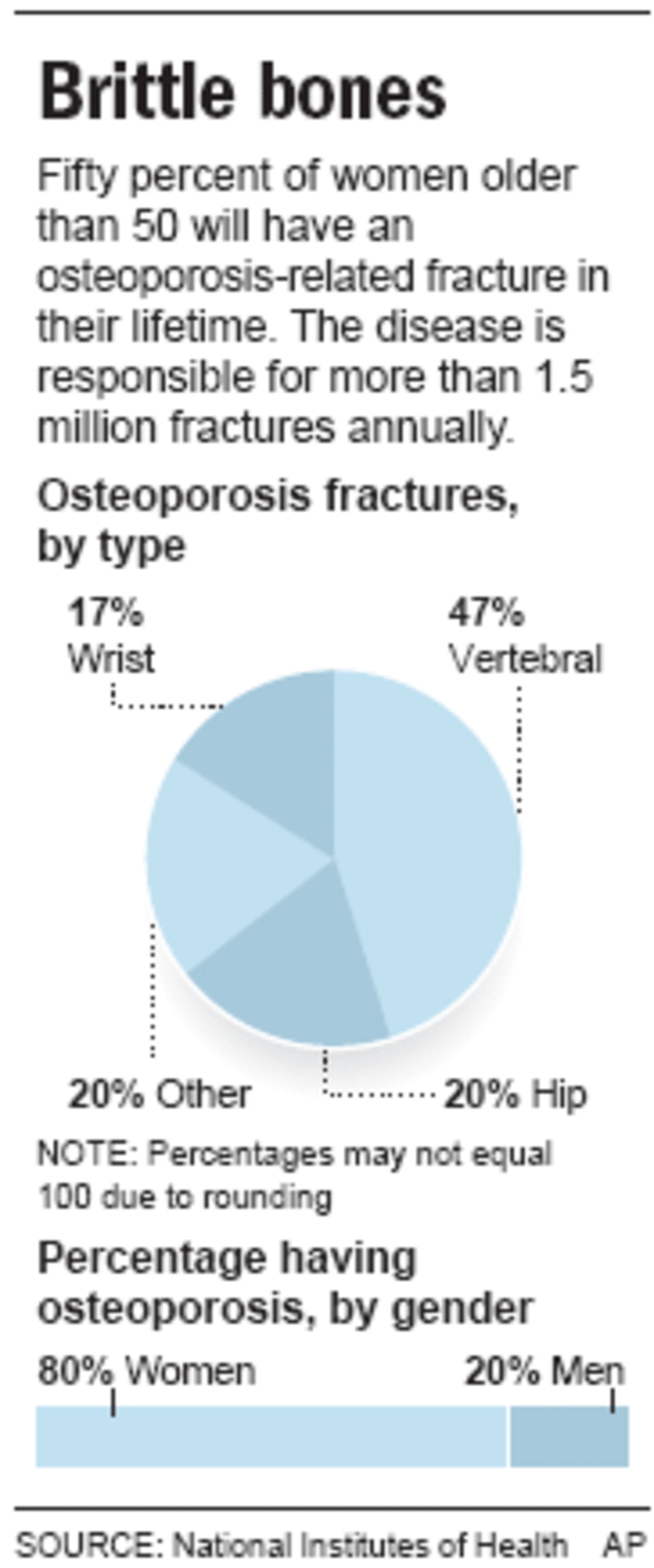
Osteoporosis touches an estimated 10 million Americans, making their bones prone to break. One of two women will suffer such a fracture in her lifetime.
For women over age 50, federal guidelines recommend 1,200 milligrams of bone-building calcium and 400-600 international units of vitamin D daily from diet and, if needed, supplements.
The seven-year study of 36,282 women ages 50 to 79 gave half the participants 1,000 milligrams of calcium and 400 units of vitamin D, while the other half took dummy pills.
However, many were also taking their own supplements before the research began, and they were allowed to keep doing so, whether they were assigned to the test group or the comparison group. These extra supplements may have helped the women stay healthy but ironically diluted the findings, since any benefit is harder to show against a backdrop of fewer fractures. Also, women in the study were taking hormone pills, likely further cutting the number of fractures.
The study showed better hip bone density in the group given supplements, but they ranked no better statistically in avoiding fractures of all kinds. However, women over age 60 reduced their chances of hip fracture by 21 percent with the supplements.
Many women sometimes missed their daily dose -- a common phenomenon in real-world testing -- but those who took their supplements most faithfully lowered their risk by 29 percent.
"We still do believe ... that maintaining an adequate calcium intake will lay the foundation for bone health," said lead author Dr. Rebecca Jackson at Ohio State University.
Dr. Bess Dawson-Hughes, a Tufts University vitamin expert who helped shape the dietary guidelines, said they should remain unchanged for now. She largely dismissed the overall negative finding.
"You put people who don't need it together with people who aren't taking it, and you find nothing -- and that really isn't all that surprising," she said.
Some researchers said the effect would have been clearer with higher doses of vitamin D, perhaps up to 1,000 units daily. The vitamin helps the body absorb calcium and promotes muscle health, reducing falls.
"We don't want to send the message to people to throw away their calcium pills, which was my wife's first reaction," said Lasser, one of the study authors.
The study did show a significant side effect with the diet supplements: a 17 percent increase in the risk of kidney stones. But several doctors downplayed that risk, saying hip fractures are typically much worse than kidney stones.
Doctors said the study suggests that women at higher risk of fracture -- whose tests show lost bone density -- likely need more than diet supplements. They may require osteoporosis drugs.
The study also checked whether the supplements might help prevent colon cancer, and the results indicated there was no benefit. That wasn't a big surprise partly because past studies had not signaled much benefit.
Still, the researchers plan to check participants in future years, because colorectal cancer can take 10 to 20 years to develop.