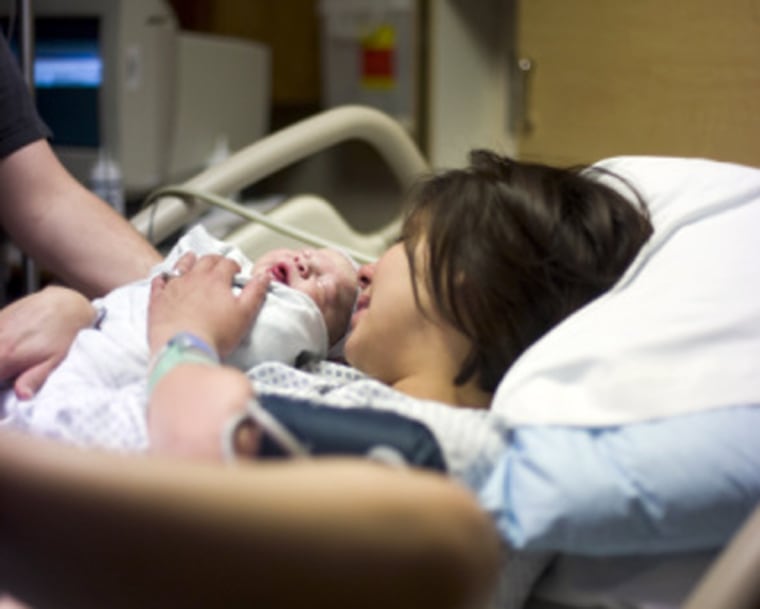
A new government study turned up some unexpected and puzzling disparities in injuries to women and babies during childbirth.
Women covered by Medicaid were less likely to be injured in childbirth than those with private insurance. Their babies, however, were more likely to experience complications, such as broken collar bones, head injuries and infections.
A similar dichotomy was revealed when the researchers compared births in urban and rural hospitals — moms did better in rural hospitals, while their babies did worse.
Overall, the news from the study was good; researchers found that childbirth complications have declined in the years between 2000 and 2006. But experts were perplexed by the disparities between the different groups of women and children.
The report, released this month by the Agency for Healthcare Research and Quality, the health services research arm of the U.S. government, doesn’t delve into the reasons for the puzzling results.
The hope is that these findings will spur other researchers to do more studies to find the underlying causes for the disparities, said the report’s senior author Roxanne Andrews, a researcher at AHRQ.
But this is the first inkling that there are some significant differences in the way doctors practice obstetrics in different types of hospitals, she said.
Overall improvements
For the new study, Andrews scrutinized data from 1,000 hospitals that are part of a national database. Included in the study were 157,000 injuries that could potentially have been prevented, Andrews said. The main injury tracked among new moms was severe tearing of the tissue between the vagina and the rectum. Generally when such a tear occurs, doctors repair it immediately. But sometimes the repairs aren’t perfect, leaving some moms at risk for serious complications such as a fistula, a condition in which the vagina and the rectum become connected.
Most of the injuries to the moms occurred during vaginal births in which instruments, such as forceps, needed be used to speed the delivery of the baby. Between 2000 and 2006, the rates of those tears dropped overall by 20 percent from 2,040 to 1,605 per 10,000 deliveries. The rate of tears when instruments were not used dropped 30 percent from 517 to 362 per 10,000 deliveries.
When researchers compared data from hospitals in rich and poor neighborhoods they found that during vaginal deliveries women from the wealthiest areas had injury rates that were 44 percent higher than those from the poorest communities.
Male infants at higher risk
The study also found that injuries were less common among black and Hispanic moms and babies than among whites. And in another unexpected association, male infants were more likely than females to sustain injuries during delivery — 15 per 10,000 newborn girls and 17 per 10,000 newborn boys.
Andrews wasn’t able to compare injuries to babies from 2000 to 2006 because hospitals changed the way that they computed those statistics in 2003. But she did determine that there were 32 injuries per 10,000 deliveries in 2006.
If the differences found by the new study turn out to be real, it’s going to take more studies to determine the causes, experts said.
You might be seeing differences in patterns of practice that are associated with the different types of hospitals, speculated Dr. Sindhu Srinivas, a specialist in high-risk pregnancy and an assistant professor of obstetrics and gynecology at the University of Pennsylvania.
One example of that could be the issue of elective cesarean section, Srinivas said. “Certain hospitals might be more likely to perform cesarean deliveries than others and this might impact the outcome. Also, different types of patients might be more likely to choose an elective cesarean.”
When C-sections aren’t as common you can end up with more cases of shoulder dystocia, a situation in which the baby’s head has passed through the mom’s vaginal opening, but then the shoulders get stuck, said Dr. Kimberly Gregory, vice chair of women’s healthcare quality and performance improvement in the department of obstetrics and gynecology at Cedars-Sinai Medical Center in Los Angeles.
Balancing the trade-off
Another factor might be differences in the way hospitals handle the trade-off between risks to the mother and her fetus during delivery, Gregory said. “There are unit ‘cultures’ that set the tone for the amount of risk doctors and hospitals will tolerate in favor of the mother or the baby,” Gregory explained. “‘Hospital culture’ is difficult to quantify, but it is very real.”
Another possible way to explain some of the findings is the prevalence of premature babies born to poor moms, said Dr. Hyagriv N. Simhan, an associate professor of obstetrics and gynecology in the division of maternal-fetal medicine at the University of Pittsburgh School of Medicine and medical director of obstetrical services at Magee-Womens Hospital.
Smaller babies are easier to deliver and far less likely to cause tears in the mom. And premature babies are more likely to be born with infections, Simhan said. Size at birth could also explain the disparity between male and female babies since boys are often born bigger, he said.
Linda Carroll is a health and science writer living in New Jersey. Her work has appeared in The New York Times, Newsday, Health magazine and SmartMoney.