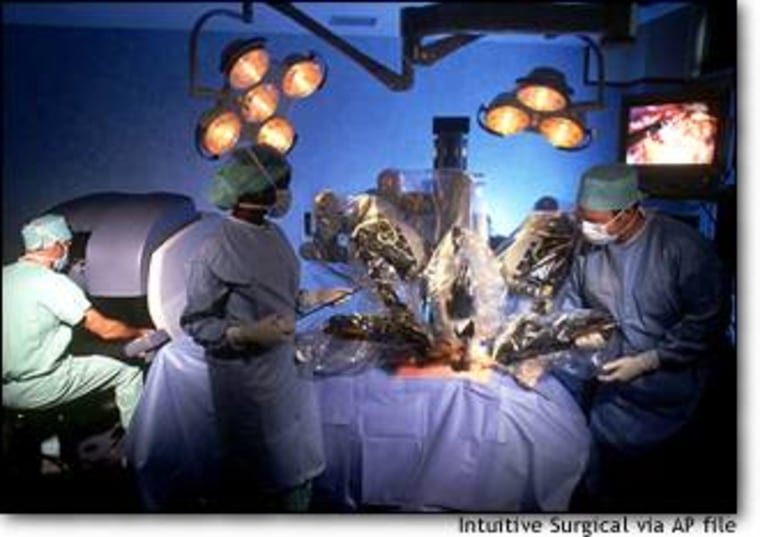
Hundreds of robots have invaded operating rooms across the globe. No, it’s not a new horror movie. Surgeons are inviting these robots to be the newest members of their teams. The minimally-invasive machines are ushering in an era of surgical precision and results unmatched by the human hand.
What do 47-year-old Scott Weikert and the 500-year old Mona Lisa have in common? They’re both alive thanks to a da Vinci. Leonardo da Vinci used unparalleled anatomical accuracy and three-dimensional detail to bring his masterpiece to life. Another da Vinci — this one a surgical robot — used the similar skills to save Weikert’s life in his battle against prostate cancer.
“There’s not a day that goes by that I don’t think, ‘Oh my God; what am I doing?’” said Dr. Mani Menon at the Henry Ford hospital system in suburban Detroit.
Da Vinci, the robot, works for Menon — a pioneer of robotic prostate removal since it was approved by the FDA less than three years ago. They’ve done nearly 600 procedures together.
That experience, and a ton of research, convinced Weikert, a construction manager and father of two from Philadelphia to travel more than 500 miles with his wife at his side to take a chance on a revolutionary approach to treating a deadly disease.
“I just felt that based on my age, and the precision of this procedure, that this was the best fit for me, as compared to the other options out there,” he said shortly before his surgery began in the operating room of the future.
Through several incisions about the diameter of a pencil, robotic instruments and cameras are plugged into Weikert. It’s a far cry from the massive incisions of traditional “open” operations.
Straight out of a science fiction movie, Menon manipulates the robotic arms from this cockpit console. He sees everything in 3D. Specialists hover around the table ready to jump in.
“Robotic surgery is a team effort,” said Menon. “It’s more like playing football than playing tennis.”
Some 200 surgeons from around the world are gathered across town, watching and waiting to get their hands on their own DaVinci.
“I’m very impressed, said Dr. David Shepherd, a Fort Worth, Tex. urologic surgeon. “I watched a gentleman before me use it and asked him if it was his first time. And he was throwing some sutures in, and he said it was, and he was doing a fine job.”
For Intuitive Surgical, creators of the million-dollar machine, this is the best possible showcase to tout the benefits for the surgeon.
“Being able to see very well under high magnification in 3D, being able to drive that camera with the robot where you need to go, having the ability to use our wristed instruments,” said Ryan Rhodes, the company’s marketing director.
And for the patient, said Rhodes, the procedure means “a quicker recovery, generally feeling better after the operation.”
Even though less than 200 machines are in operating rooms worldwide, physicians say word of mouth and the Internet are fueling demand.
“Some of what’s happening in robotics is that it’s sexy,” said Dr. Wayne Poll, a surgeon in private practice in Columbus, Ohio. “And patients not really knowing the difference — just wanting the most advanced technology.”
High tech, yes. But there’s nothing sexy about prostate surgery — robotic or otherwise. Other procedures where da Vinci is doing its clearing and cutting include: the gastric bypass — a stomach stapling procedure — made famous by a host of celebrity patients. It’s also being used to repair the esophagus in patients with chronic heartburn.
And critical to Intuitive’s future is a green light from the FDA for heart bypass surgery. That would mean a lot of green.
And as the doctor never touches the patient, the traditional boundaries of the operating room walls are melting away, allowing surgeons to operate da Vinci from across the globe.
Menon thinks the “sky’s the limit” for robotics in the operating room. And doctors, like airline pilots, will earn their wings on simulators. So that when a surgeon sits down for their first operation, they will have done it hundreds of times in virtual reality.
“You’ll be able to set standards,” said Menon. “And say you can only operate on a human when you’ve done these procedures at this speed and this precision, and its perfectly measurable.”
But for all the potential — cost and upkeep remain the biggest barriers. The $1 million purchase price for the machine is just the beginning. Annual maintenance and training costs hundreds of thousands of dollars.
That’s money that hospitals are hard pressed to spend, as insurers ponder whether the technology is “reasonable and necessary” and, if so, how much should they reimburse.
“Too often, hospitals have to make a choice that if they’re going to use a new technology, they may lose money on it,” said Pamela Bailey, who runs the nation’s largest trade association for medical device makers.
Back home, one week after surgery, Weikert was already working. The typical prostate patient suffers six to eight weeks of debilitating pain.
“The recovery has been miraculous,” he said. “I have no pain associated with it.”
He’s back on his feet and walking two miles a day, while others would be bedridden. And he’s helping medical trailblazers deliver the future, now.
(CNBC's Steve Lewis contributed to this report.)