The “magic mushroom” drug psilocybin can help cancer patients relax and feel less distressed about their disease, two teams of doctors reported Thursday.
The drug eased anxiety and depression in 80 percent of the patients who took it in the studies, and many described their one-time sessions as ranking among the most meaningful experiences of their lives.
While the drug is clearly not for everyone, it’s worth testing under carefully controlled conditions in more patients, the researchers concluded.
“We found that a single dose of psilocybin immediately reduced symptoms of depression and anxiety in patients that had advanced cancer and life-threatening forms of cancer,” Dr. Stephen Ross, director of addiction psychiatry at New York University’s Langone Medical Center, told NBC News.
Gale Cowan was one of them. The 73-year-old New York adult literacy teacher has been dealing with breast cancer on and off since 2003. She knows it’s likely to kill her.
“It was sort of like this deep sense of dread, that this cancer was stalking me,” she told NBC News. “And every time I think I beat it back, it would catch up with me again,” Cowan added. “It was coming back every two or three years.”
It’s a common feeling, Ross said.

“Forty to 50 percent of patients with cancer will have some diagnosable anxiety or depressive disorder,” he said.
Cowan had tried LSD in her 20s and so didn’t feel many doubts about joining a clinical trial of psilocybin.
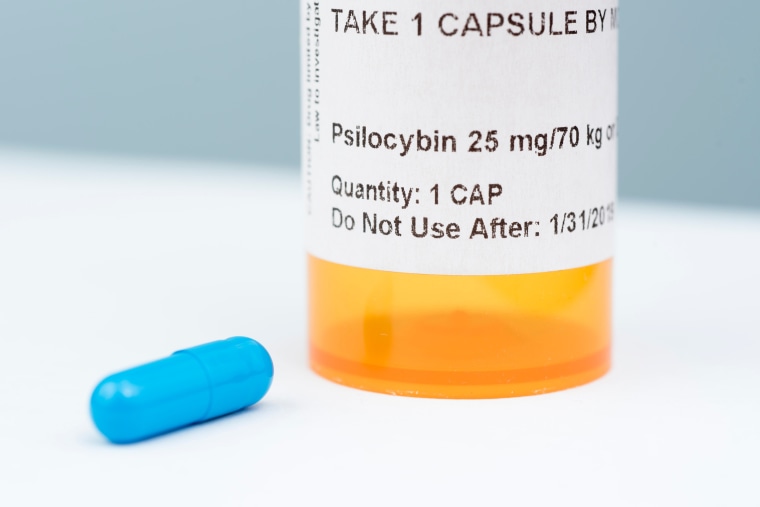
The researchers delivered the drug – a synthetic version of the active ingredient of the mushrooms – in a carefully controlled setting, with therapists on hand, soothing music and plenty of objects for the volunteers to look at and touch.
“It starts off more like the things that I was seeing were heightened,” Cowan said. “Even like that lamp --all of a sudden you know the texture of the shade.”
“I felt this connection with everything."
She noticed the upholstery on the couch and the leaves on the trees outside the window. “And they had some lovely art objects -- statues and pottery things and books. They had flowers -- very nice.”
Cowan said the experience – it lasted a few hours – made her feel like she was part of something bigger.
“I felt this connection with everything,” she said. “There's something that I go into and become a part of and that's pretty cool. My experience tells me that it's not a big nothing after I'm gone.”
Another patient, Rob Sweeney, described a similar feeling. “I was floating on this immense expansive infinite sea of strength and beauty,” he said. “There was no difference between that infinite sea and me.”
The calm feeling stayed with her, Cowan said.
“Every night when I get in bed, and the lights (go) out, I find that I have a smile on my face even if I've had a really stressful day,” she said.
“I am lying there with a smile on my face,” she added.
The team at NYU tested 29 patients. Another team, at Johns Hopkins University, tested 51. Both had similar results, reported in the Journal of Psychopharmacology.
“I would be worried that cancer patients would look at this and think ‘I'm going to go out, get magic mushrooms and do it at home’. No, that's not the safe way to do it.”
"The most interesting and remarkable finding is that a single dose of psilocybin, which lasts four to six hours, produced enduring decreases in depression and anxiety symptoms, and this may represent a fascinating new model for treating some psychiatric conditions," says Roland Griffiths, a professor of behavioral biology at the Johns Hopkins University School of Medicine.
"Before beginning the study, it wasn't clear to me that this treatment would be helpful, since cancer patients may experience profound hopelessness in response to their diagnosis, which is often followed by multiple surgeries and prolonged chemotherapy," Griffiths added in a statement.
"I could imagine that cancer patients would receive psilocybin, look into the existential void and come out even more fearful."
None did in the trials, although the good effects did not always happen immediately.
“Initially it was absolutely terrifying. I was just terrified,” said Dinah Bazer, one of the NYU volunteers. But then the drug allowed her to visualize her anxiety about a grim cancer diagnosis.
“I saw my fear. The fear was gone,” she said.
“They markedly looked different and better,” Ross added.
The studies are part of a growing movement to examine illegal recreational drugs to see if they can help specific medical conditions. Marijuana and cannabis are the most commonly tested. The Food and Drug Administration just okayed a large trial of Ecstasy, known chemically as methylenedioxymethamphetamine or MDMA, to treat veterans with post traumatic stress disorder or PTSD.
There’s actually nothing new about trying mind-altering drugs to treat psychiatric conditions.
“When Albert Hoffman discovered the remarkable mind-altering properties of lysergic acid diethylamide (LSD) in 1943, he didn’t have much trouble persuading his bosses at the pharmaceutical company Sandoz (now part of Novartis) that this drug would play a very important role in understanding the nature of mental illness and potentially providing a very novel approach to their treatment,” David Nutt of Imperial College London and editor of the Journal of Psychopharmacology, wrote in an editorial accompanying Thursday’s studies.
“Through the 1950s and 1960s, Sandoz supplied medical LSD in the form of Delysid that was studied in hundreds of trials in thousands of patients. The U.S. government via the National Institutes of Health funded more than 130 grants in this field.”
That stopped in 1970, after so many people started taking drugs such as LSD recreationally and had “bad trips” that worsened psychosis and schizophrenia. The Drug Enforcement Administration strictly limits the use of psilocybin.
“They really were misused by many Americans and these are not drugs that should be used recreationally,” NYU’s Ross said.
“To many people brought up in the Reagan drug war era with the ‘drugs fry your brain’ message, psilocybin may seem a strange and possibly even a dangerous drug treatment of serious mental illness,” Nutt added.
“The thing that I would be most upset about from this research would be if people in the public thought ‘this is great. This is a cure. This is going to help everyone’."
But he said it has few physical side effects.
Ross said he’s been inspired to try to help advanced cancer patients since he saw a stark contrast between what doctors often do and what good end-of-life care can look like.
“When I was a medical student and an intern, I really saw bad death. I saw people getting chemotherapy on their deathbed and doctors really not trained to help patients in the final part of their lives,” Ross said.
“I realized that doctors are just poorly trained in how to help a dying patient.”
Ross stresses that the patients are treated in a controlled environment, with therapists on hand. Volunteers were screened for any family history of mental illness such as psychosis, and tested for use of other drugs such as cocaine.
“The thing that I would be most upset about from this research would be if people in the public thought ‘this is great. This is a cure. This is going to help everyone’,” Ross said.
“I would be worried that cancer patients would look at this and think ‘I'm going to go out, get magic mushrooms and do it at home’. No, that's not the safe way to do it.”

