I had barely begun to digest my diagnosis of prostate cancer when a whole new plate of terms was thrust before me: radical prostatectomy, brachytherapy, watchful waiting, proton beams, cryotherapy.
Welcome to the prostate cancer treatment buffet, where the presence of so many chances for a cure seems too good to be true and, for me, it is. Because there’s no consensus in the medical community on a gold standard treatment for prostate cancer, a patient must choose his own. Welcome to hell.
While the biopsy was painful and nerve-wracking, and the news that I had cancer invoked fear, having to pick my own treatment has easily been the most agonizing part of this ordeal so far. I hope that continues to be true and that I won't have to make any choices about what to do next. It can only get worse.
It’s hard to admit these feelings because they make me feel like an ungrateful whiner. Instead of cowering before a cornucopia of good treatment options, shouldn’t I be celebrating all that modern medicine has to offer prostate cancer patients? I sure as shooting wouldn’t want to have something for which the doctor merely tells you to pray.
But that thinking doesn’t help silence the gathering electrical storm inside my head. After attacking books and studies and Web sites with gusto at first, the mental thunder and lightning has only grown louder. For every choice, there are heart-warming success stories and sad disappointments.
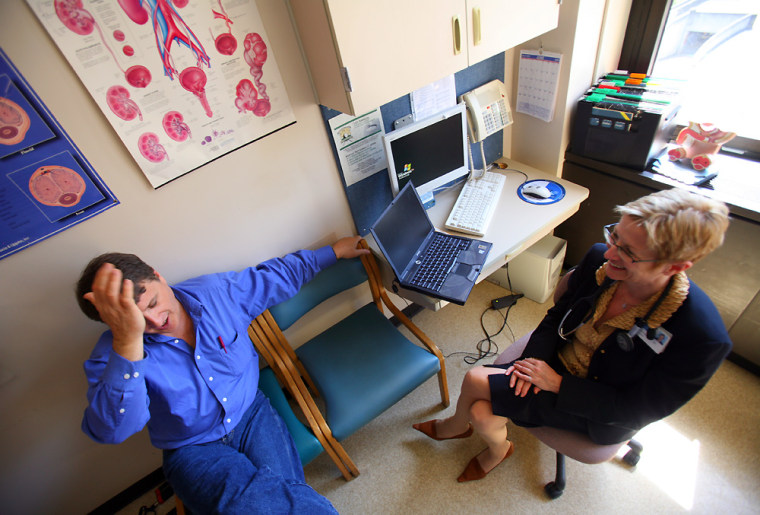
On a big sheet of flimsy paper that covers a padded table in a bright examination room, the doctor who diagnosed my cancer, Christopher Porter, a urologist at Virginia Mason Medical Center in Seattle, outlines my situation with a blue ballpoint. He sketches my bladder, urethra and prostate, and goes over the data from my tests. My latest PSA reading is 6.88, the cancer is Gleason grade 6 and my clinical stage is T2a. Those numbers point to a case of cancer that is most likely confined to the prostate gland. It almost certainly hasn’t spread to my seminal vesicles, bones or lymph nodes.
5 options, 5 paralyzing decisions
“Good risk,” he scrawls in the margin and underlines it. In his view, that means I have five reasonable choices: watchful waiting, often going by the term active surveillance these days; surgery done one of two ways; or one of two radiation treatments.
Porter makes it clear that although his hospital is participating in a clinical trial of active surveillance, that’s the one choice he would not enthusiastically support for a guy my age, 49. From my reading, I already agree. Numbers like mine indicate cancer that's probably not racing to spread, but would cut my life short if left untreated. As long as I will need to treat it at some point, I decide to do it now.
Also from my own research, I have rejected some treatments that Porter doesn’t even mention: proton beam therapy and cryotherapy, to name two. While both are clearly good treatments for many patients with prostate cancer, I can find no data that show them to be better.
When it comes to surgery vs. radiation, Porter is quick to admit his bias toward surgery. Urologists are surgeons. But, with a caveat, he is also quick to say that data show radiation therapies to have about the same effectiveness in curing cancer. The caveat is that radiation doses and techniques have shifted in recent years so the track record, while as good as surgery, is not as long.
If I go with surgery, known as a radical prostatectomy, Porter could cut me open the old-fashioned way, leaving an 8-inch incision from my belly button to my pubic bone. Or he could use a robotic assistant known as the Da Vinci. The robot would deploy a remote camera and surgical devices through five small holes to take out my prostate. The main benefits of the Da Vinci are that the surgery is gentler on the body and recovery times may be faster.
But either way, I'd still leave the hospital trailing a catheter and a pee bag.
Consulting with some of Porter’s colleagues who perform radiation treatments, and from my own reading, I decide that were I to choose radiation therapy, I would try brachytherapy, which involves injecting tiny radioactive "seeds" directly into the prostate. The radiation oncologists say they believe the cure rate is as fine as any option and side effects are much less of a risk than when radiation is externally beamed at the prostate.
So what about those side effects? I’m happy to know how great my odds are at beating cancer, but I am hoping for more. I’m a Baby Boomer American male. Like many others in my generation, I don’t merely want a lot. I want it all. So of course I want my cancer cured, I want it cured now, and I want it to be as convenient as possible. Down the road, I don’t want any telltale wet spots on my khakis and I want to awaken every so often with a raging, natural, er, you know.
My research and conversations with prostate cancer survivors convince me that the risk of bad incontinence from either surgery or radiation is not huge. Porter says his results are in the high 90 percent range for men to be free of any serious issues — and protective undergarments — a year after surgery. All of the surgery patients with whom I have spoken, save one, agree.
Potency is a whole other story. Not too many years ago, impotence was an accepted cost of all prostate surgery. But in the ’80s, surgeons found the nerves that control Mr. Happy and perfected “nerve-sparing surgery” to save them. This is the procedure Porter uses. He believes that three-quarters of patients my age or younger who have surgery at his hospital regain satisfactory potency within a couple years. While he believes that half of all radiation patients eventually become impotent, he cannot separate the stats by age. His radiation colleagues believe that for a guy my age the impotency risk with radioactive seeds is considerably less but can’t cite any definitive studies.
One reason that it’s harder to track the differences between surgery and radiation is that if surgery ends your ability to achieve an erection, it happens immediately. With radiation, it can take two to three years.
I leave Porter’s office nowhere near ready to make a choice. I feel like there is only one right decision and if I blow it, I'll regret it for the rest of my life. The electrical storm crackles and pops.
I split from my wife of 23 years not too long ago and now am in a fairly new relationship. This has been a very difficult time for my girlfriend, too; studies show that the emotional toll of prostate cancer is frequently higher for the patient's partner than for the patient himself.
Would you rather...?
The sex issue is heaviest on my mind. Once again, I find myself feeling a bit ashamed for dwelling on it so much. Strong advice from Dr. Ksenija Stefanovic, one of Porter's urologist colleagues who will advise and treat me for any sexual complications, is not to base my treatment decision on my hopes for the best outcome in bed.
First and foremost, take your best shot at curing the cancer, she counsels. When it comes to sex problems, "there are no guarantees" with any of the choices but there are many ways to try to solve them.
Still, I feel like my treatment options have become a bizarre revenge for all those drunken hypothetical debates I joined as a young man around the campfire: Rather be blind or confined to a wheelchair? Deaf or lose your sense of taste? Live longer and screw less, or vice-versa?
I can’t say that my anxiety over this issue is a conscious fear of losing my “manhood.” I don’t think I like sex so much because it makes me feel powerful and manly. I can always take up weight-lifting or buy an F-350 with a Powerstroke diesel. I think I like sex so much because I just like sex so much. I like it like I like seeing, walking, hearing, tasting and breathing.
Yes, there’s fun and intimacy to be had in bed without erections. But when talk turns to sex among women, I’ve heard that while debate can get fast and furious over whether size matters, there’s never any argument over hard vs. soft. The talk of all the new remedies for erectile dysfunction rings as hollow as the promise of crutches to a prospective amputee.
On a hopeful note, some couples insist that the whole experience of sex without erections is just as satisfying as with them, if quite different. But my own hopeful note is that I don’t have to find out.
MSNBC.com writer Mike Stuckey was diagnosed with prostate cancer in April. He will chronicle his battle in "Low Blow," a series appearing every other Wednesday. In the next installment, Mike chooses a treatment.